
Common warts are a routine concern in pediatric practices, often brought in by children or their parents for removal. With a handheld, aerosol-based cryosurgery tool, treatment can now be performed quickly, in just seconds.
Improve patient comfort and satisfaction with weekly advice
delivered directly to your inbox.

Do not spray in eyes. Over spraying may cause frostbite. Freezing may alter skin pigmentation. Use caution when using product on persons with poor circulation. The thawing process may be painful and freezing may lower resistance to infection and delay healing. If skin irritation develops, discontinue use. CAUTION: Federal law restricts this device to sale by or on the order of a licensed healthcare practitioner.
Apply only to intact oral mucous membranes. Do not use on genital mucous membranes. Consult your pediatrician when using on children 4 years old and younger.
Published clinical trial results support the use in children 3 years of age and older. Ethyl chloride is FLAMMABLE and should never be used in the presence of an open flame or electrical cautery equipment. Use in a well-ventilated area. Intentional misuse by deliberately concentrating or inhaling the contents can be harmful or fatal. Do not spray in eyes. Over application of the product may lead to frostbite and/or altered skin pigmentation. Cutaneous sensitization may occur, but appears to be extremely rare. CAUTION: Federal law restricts this device to sale by or on the order of a licensed healthcare practitioner.
By: Kathleen Orellana | On: May 13, 2026

Common warts are a routine concern in pediatric practices, often brought in by children or their parents for removal. With a handheld, aerosol-based cryosurgery tool, treatment can now be performed quickly, in just seconds.
By: Kathleen Orellana | On: April 16, 2026

While implementing patient comfort measures may only take a few minutes, they can pay big dividends when it comes to patient satisfaction survey results. Reducing patient discomfort and providing a better patient experience can be as easy as using one of these three nursing techniques for pain management.
By: Kathleen Orellana | On: March 16, 2026
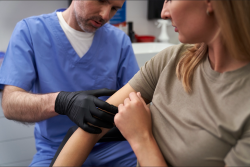
Is liquid nitrogen or Cryo Professional portable cryosurgical system the best way for clinicians to treat benign lesions or common dermatologic issues?
The first consideration for any primary care practice, urgent care, or mobile clinic is choosing a treatment solution that delivers the best clinical outcomes.
Since time, space, and cost are always considerations, the right solution must also be easy to use, portable, and affordable.
This means understanding how both solutions meet clinical efficacy, workflow, storage constraints, staff training, and operational overhead demands.
By: Kathleen Orellana | On: February 24, 2026

Keeping geriatric patients comfortable can be challenging, especially when they have multiple health issues. Ensuring patient comfort is crucial for patients and their families, and it should also be a priority for your hospital, as it significantly impacts patient satisfaction.
Instituting a comprehensive training program supporting comfort solutions for geriatric patients can help your staff provide an even higher level of care. Whether you use formal training sessions or lunch-and-learns, ongoing training should be a priority. Here are a few tips to get you started:
By: Kathleen Orellana | On: February 20, 2026

By taking proactive measures to improve patient retention, you can inspire long-term relationships with each and every patient. Here are our tips to increase patient retention rates in your practice:
By: Sue Zagula | On: March 20, 2025

The debate over Full Practice Authority (FPA) has resurfaced in recent years. Exclusive licensure authority allows nurse practitioners and others to practice independently under the guidelines set by the state board of nursing. Proponents say it can increase access to care, improve health outcomes, and reduce costs, while critics express concerns about the quality of care and patient safety.
By: Sue Zagula | On: March 14, 2025

The concept of Full Practice Authority (FPA) for advanced practice registered nurses has become a topic of frequent discussion in recent years as hospitals and primary care providers look for new ways to deal with rising costs, recruitment and retention challenges, and increasing administrative demands.
By: Sue Zagula | On: September 19, 2024

For patients, a blood draw can be more than just a routine medical procedure. The fear associated with anticipated pain can overshadow the medical necessity, leaving patients feeling anxious and dreading future appointments. This can lead to needle phobia and even avoidance of essential care in the future.
By: Morgan O'Leary | On: May 31, 2023
-min-1.jpg)
Patient comfort is a known factor that can help or hinder medical outcomes.
When pediatricians and pediatric nurses speed through appointments, patients’ fears may increase, their cooperation may be impaired, and they may even experience more discomfort. Having a child life specialist on board can add extra support to both the child, child’s family, and medical team to ensure that patient trust and comfort, critical components of trauma-informed care, remain at the forefront.
See how Gebauer’s Pain Ease topical anesthetic skin refrigerant can improve patient comfort in pediatrics. Download the guide.
By: Sue Zagula | On: April 6, 2023
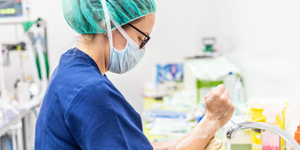
During the beginning of the COVID pandemic, when hospitals were overwhelmed and personal protective equipment was in short supply, healthcare-associated infections (HAIs) significantly increased after declining for years. Now, as more people succumb to “pandemic fatigue,” many have seemingly become less cautious about getting sick and are abandoning preventative behaviors, such as wearing masks and social distancing. Hospitals are beginning to fill up again as the flu, COVID, RSV, and other infectious diseases spread. Now is a good time for hospitals and private practices to review infection prevention strategies and be prepared for whatever the future may bring. Here are five strategies to get you started:
By: Sue Zagula | On: March 15, 2022

We often hear nurses described as dedicated, empathetic, trustworthy, and even heroic — especially in the wake of the COVID-19 pandemic. But while there are plenty of adjectives we can attribute to these life-saving professionals, the job often seems too complex and dynamic to capture in one, easy-to-read definition.
By: Sue Zagula | On: February 24, 2022

For nearly two decades, nurses have ranked No. 1 in Gallup’s annual poll of the most honest and ethical professions, surpassing doctors, grade-school teachers, and even clergy. And, as the pandemic continues on, public perception of nurses has only improved.
By: Sue Zagula | On: January 27, 2022

Travel nursing is an essential component of nearly every healthcare system. When there’s a shortage of nurses within a region or facility, these adventurous healthcare pros step in to fill the gap and ensure patients get the care they need.
By: Sue Zagula | On: November 2, 2021
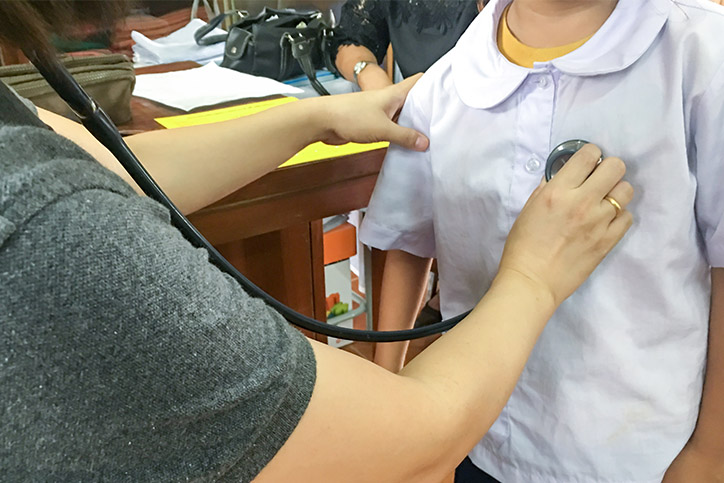
Most of us can recall at least one encounter with a school nurse during our childhoods. Perhaps your school nurse was the comforting presence you needed when you suddenly came down with a raging fever, or put your mind at ease while patching up a playground injury. But while these experiences are certainly common, school nurses do much more than take temperatures and slap bandaids on scraped knees. And their job is ever-evolving.
By: Sue Zagula | On: October 20, 2021
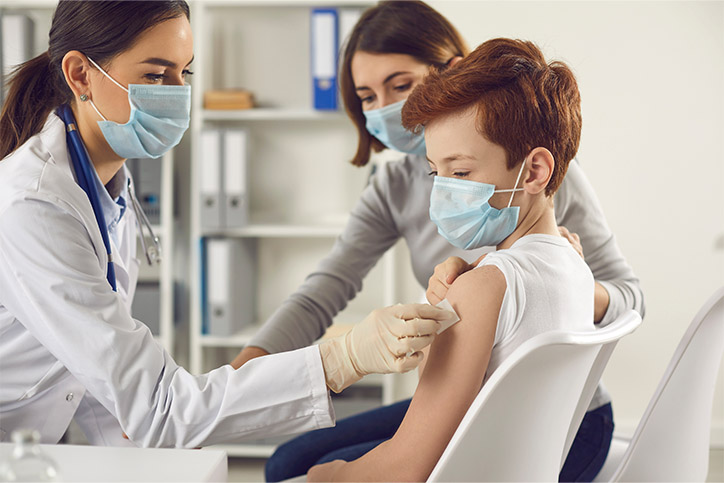
Healthcare has a long way to go in assisting youth and their families move from the pediatric world to the adult healthcare team. According to the 2017/2018 National Survey of Children’s Health, several families report many barriers to transition from pediatric to adult healthcare, including not being comfortable moving to a new doctor, finding a doctor that they can talk to, understanding how to make appointments or how to determine insurance coverage.
By: Sue Zagula | On: September 15, 2021

The transition from late teens to early adulthood is rife with challenges, transformations, and new experiences. It’s a time when adolescents leave behind the comforts of childhood and begin embracing the freedom and responsibility of being an adult. From going away to college and choosing a career path to handling finances and living away from home, it’s all a bit overwhelming. And navigating healthcare adds yet another layer of complexity to this life phase.
By: Bethany Nock | On: August 17, 2021

As a clinician, you’re accustomed to fielding patients’ questions and managing skepticism over various treatments. In some cases, a patient’s hunger for information is a positive sign that they’re invested in their health and will be dedicated to their prescribed care plan. But, when patients have the wrong information, it can lead to noncompliance or full-on refusal of care.
By: Bethany Nock | On: July 8, 2021

For much of modern history, cultures have used handshakes as a greeting and a symbolic gesture to close business transactions. But, since the COVID-19 pandemic began in early 2020, handshakes have almost entirely disappeared in favor of elbow bumps and socially distanced waves. Now, even as more people become vaccinated and are once again connecting in person, many of us are still a little leery of touching each others’ hands.
By: Bethany Nock | On: June 8, 2021

Working as a nurse is one of the most rewarding yet demanding and often overwhelming career paths in the professional world. In many cases, nurses rely on peers and external support systems for encouragement and advice — but some questions and challenges require more experienced insight. And that’s where a nurse mentor can be most beneficial.
By: Bethany Nock | On: May 10, 2021

For nineteen years, Americans have ranked nursing as the No. 1 most honest and ethical profession, according to an annual Gallup poll. Nurses outrank physicians, teachers, pharmacists, judges and even members of the clergy.
The integrity of nursing is also one of the few things Americans across the political spectrum agree upon, with democrat and republican respondents choosing nurses as No. 1 in near-equal measure.
The bottom line is people from all walks of life trust nurses with their lives. But what is it about nurses that foster such a deep sense of faith and confidence? In honor of nurses’ week, we’re delving into a few reasons people consistently rank nursing as the most trusted profession in the country.
By: Bethany Nock | On: April 27, 2021

The past year has been one of the bleakest, most harrowing, and emotionally exhausting periods in recent history — particularly for our nation’s frontline healthcare workers. But, despite several months of unspeakable challenges and an uncertain future, these professionals have continued showing up, often risking their own wellbeing to care for those in need.
From providing palliative care to patients with severe cases of COVID-19 to assisting women giving birth and helping treat all manner of conditions amidst the deadly pandemic, these healthcare heroes have given a new meaning to the term patient experience.
By: Bethany Nock | On: April 15, 2021

Contrary to many beliefs, children are not just mini-adults. Children of all ages are continuously developing physically, psychologically and socially. Whether they are 6 or 16, they react differently than adults when confronted with challenges and changes in their routines. This is especially true when children enter the hospital. Because they may not fully understand what is happening to them, they may become resistant to the care offered. At the same time, family members may be anxious and may unknowingly add to the child’s fears.
By: Bethany Nock | On: March 9, 2021
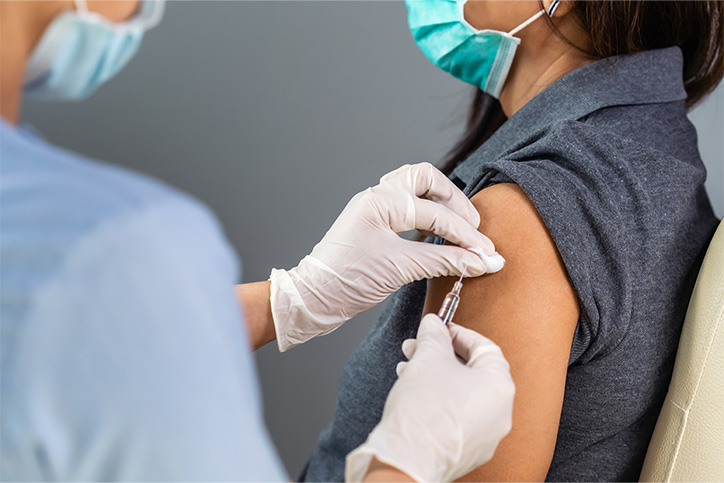
The news is covered with the many challenges associated with mass vaccine distribution and administration. Unfortunately, the words efficiency and comfort are not making the headlines related to this undertaking. In this blog we will breakdown how efficiency is critical to maximize patient output, and how keeping patient comfort at the forefront can help fuel efficiency goals.
By: Bethany Nock | On: February 23, 2021

Dealing with hospitalized pediatric patients can be both challenging and rewarding. Depending on the stage of development the child is in, are required to manage his or her hospital stay. But just paying attention to the needs of the child is not enough. Parents and loved ones often show signs of stress and anxiety which can be mirrored in the child’s behavior. Ignoring the child’s loved ones can result in increased feelings of stress and anxiety for the entire family. And this can result in frustration and taxing situations for you!
By: Bethany Nock | On: January 5, 2021

Are all nurse mangers leaders? Although leadership and management monikers are often interchanged in conversation, the reality is that being a leader requires very different skills than that of a manager. This article discusses those differences and explores what they can mean to you as a nurse.
By: Bethany Nock | On: November 17, 2020

The Institute of Medicine’s The Future of Nursing: Leading Change, Advancing Health, published in 2010, offers the nursing workforce a map to follow to keep up with the changing needs of the diverse patient population. One of the four main goals included in this report is that nurses should strive to achieve higher levels of education. Two ways that can be achieved is through advanced practice status, such as Certified Nurse Practitioner, or through specialty nursing certifications, such as CEN (Certified Emergency Nurse). According to a 2020 survey of nursing professionals, about 56% of men and 49% of women are considering pursuing higher education, certification or training.
By: Bethany Nock | On: October 13, 2020

The Magnet Recognition Program®, developed by the American Nurses Credentialing Center (ANCC), awards the designation of “Magnet Hospital” to organizations that demonstrate excellence in nursing, nursing innovation and patient care. Currently, only 461 hospitals in the U.S. have earned this distinction, according to data from Duquesne University School of Nursing, and out of the top 20 Best Hospitals Honor Roll from 2017 - 2018, 17 are Magnet Hospitals.
By: Bethany Nock | On: September 23, 2020

No one goes into nursing expecting a cakewalk. This profession is not only physically demanding, but mentally and emotionally taxing, too. You’re expected to be strong in the face of suffering and tragedy while also showing compassion and empathy, and straddling this line can be difficult.
By: Bethany Nock | On: September 15, 2020

Because many conversations between healthcare professionals and patients discuss serious issues concerning patient’s health, it is extremely important to make sure that the practitioner uses appropriate communication skills. These discussions should always be kind and informative. You should maintain eye contact, deliver the information with respect and care and be open to the other’s point of view.
By: Bethany Nock | On: August 25, 2020
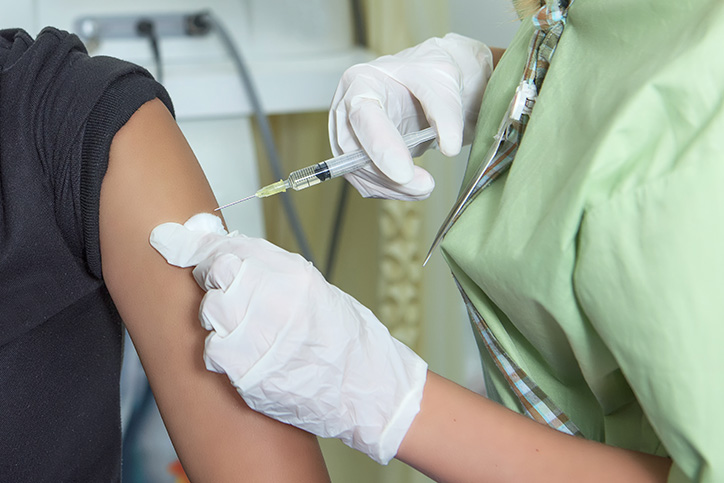
Healthcare protocols are changing continuously during these times of the global pandemic. One thing that retains its importance is keeping patients up to date on their immunizations. The Center for Disease Control and Prevention has stated that “ensuring immunization services are maintained or reinitiated is essential for protecting individuals and communities from vaccine-preventable diseases and outbreaks and reducing the burden of respiratory illness during the upcoming influenza season”.
By: Bethany Nock | On: August 18, 2020

Nursing can be an extremely rewarding career path; however, the daily grind of the job can wear individuals down over the course of time causing feelings of exhaustion, depression or even reduced self-confidence. A 2018 Gallup study revealed that two-thirds of full-time workers feel the effects of burnout at their job, showing this is a common, yet undesirable state of affairs.
By: Bethany Nock | On: August 4, 2020

One of the goals of the 2010 Institute of Medicine’s (IOM) Future of Nursing report was to increase the leadership and organizational involvement of nurses at all levels. As a nurse, you can make a difference and increase your voice and leadership skills by being a valuable member of a hospital committee.
By: Bethany Nock | On: July 21, 2020

It is rewarding and fulfilling to contribute to successful outcomes with a group of people. Being part of a team helps us achieve greater goals than we can alone. This is especially true in healthcare when the stakes are usually high, and the goals are substantial. Being part of a positive team versus one that is negative can make a world of difference. Hopefully, you have participated in teams that have been so gratifying and productive that you want to work with those people again or replicate that success to other team environments in your life. Conversely, many of us may have participated in a group or committee where some of the members did not participate, say or did things to only “stir the pot” or sabotaged the work of others. These can be frustrating experiences and can decrease morale and productivity.
By: Bethany Nock | On: July 7, 2020

Many adults experience at least some level of anxiety when preparing for a needle procedure — but for young patients, it can be especially traumatic. Often, children’s apprehension originates from a fear of bodily harm, their lack of control over the situation, and their lack of experience undergoing venipuncture.
By: Bethany Nock | On: June 16, 2020
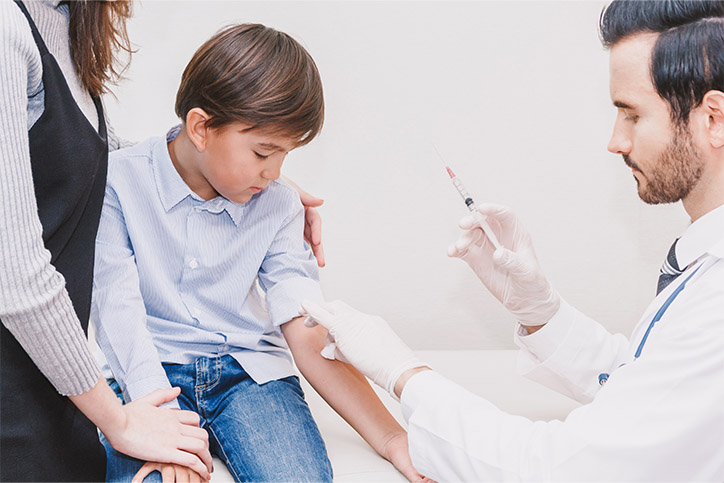
When many people think of taking a child to the doctors, even if it is for a routine check-up, the words “fast” and “efficient” are probably not in their top-ten list of adjectives to describe the experience. Although there is an unimaginably long list of variables to consider when keeping a pediatric patient (especially younger ones) calm during the visit, there are some fairly manageable techniques and changes you can consider implementing into your routine that may help smooth out the experience.
By: Sue Zagula | On: May 7, 2020

Stress is a normal part of life. In moderation, stress can be good for you! It affects everyone, no matter what your profession, if you are on the job or at home. According to a study printed in a National Institute of Health (NIH) publication, healthcare professions are among the most stressful professions. Healthcare professionals are responsible for the care given to many generations of patients from birth to geriatrics. There are many decisions to be made while giving that care, and the actions (or lack of actions) taken by clinicians can have life-changing effects on their patients. Definitely stress inducing!
By: Bethany Nock | On: April 23, 2020

The world has changed in many ways over the last couple weeks and months. Some of those changes are for the better, some are inconvenient or frustrating and some are temporary.
By: Bethany Nock | On: March 10, 2020

The month of March is all about Child Life. Child Life Specialists, that is. These men and women are often the secret ingredient to many successful pediatric departments. As we recognize these professionals this month, let’s shine the spotlight on three reasons why Child Life Specialists are so important to your facility:
By: Bethany Nock | On: February 20, 2020
By: Bethany Nock | On: January 16, 2020
By: Bethany Nock | On: December 17, 2019
By: Bethany Nock | On: November 12, 2019
By: Bethany Nock | On: September 24, 2019
By: Bethany Nock | On: August 27, 2019
August is National Immunization Awareness Month (NIAM), an annual observance of the importance of vaccinations — which are especially critical during the busy back-to-school period and before the onset of flu season. But as a healthcare professional, you know it’s crucial to cultivate recognition for the value of immunizations all year round.
By: Bethany Nock | On: July 17, 2019

Experienced nursing professionals know that providing a positive patient experience is critical to driving better outcomes. But this can be especially challenging when you’re faced with circumstances beyond your control — like issues with your electronic medical records (EMR) system, for example.
By: Bethany Nock | On: May 21, 2019

Firefighters, police officers, construction workers — most people aren’t shocked to learn these roles are among the most dangerous professions. But what about nursing?
While many health care professionals face severe and even life-threatening workplace hazards regularly — this is especially true for nurses. RNs have some of the highest illness and injury rates in the healthcare and social assistance sector, according to data from the U.S. Bureau of Labor Statistics.
By: Sue Zagula | On: May 7, 2019

Over the past few years, healthcare professionals have begun using the term patient-centered care to describe a growing number of processes and activities. Because the term has become more pervasive, it can be challenging to decipher exactly what patient-centered care means, what it encompasses and, most importantly, how you can create a more patient-centered experience within your healthcare organization.
By: Sue Zagula | On: February 28, 2019

As an experienced healthcare professional, you know providing a positive experience is crucial for earning a patient’s trust, regardless of their age. But when it comes to treating pediatric patients who are just beginning to associate the hospital environment with feeling pain, establishing trust is even more critical.
By: Bethany Nock | On: February 12, 2019

We have enjoyed being a successful family owned and operated business for 120 years. Over that time, a variety of products have been developed, launched and successfully utilized in the marketplace. Some have stayed, and some have moved on. Today, we are excited to celebrate one of our most successful product lines, Gebauer’s Pain Ease®. This product is instant, non-drug, non-flammable and, best of all, easy to use. It’s no wonder it continues to be a fast-growing favorite.
By: Sue Zagula | On: January 28, 2019

Since the early 2000’s, lack of handwashing has been targeted as a main cause of spreading infections. Over the years, Joint Commission has required organizations to develop and implement hand hygiene programs. As of January 1, 2018, the Joint Commission has decided to take another step to ensure hand hygiene is top of mind while providing direct patient care. Surveyors will now cite a deficiency to a hospital if they see any individual failing to perform hand hygiene.
By: Sue Zagula | On: November 14, 2018

We loved seeing so many nursing professionals at the 2018 ANCC National Magnet Conference in Denver Colorado on October 24-26, 2018. The record-breaking crowd of over 10,000 healthcare workers included nurses, unit managers, chief nursing officers, directors, educators and researchers. The MAGNET conference brings nurses together to celebrate their MAGNET journey and improve their nursing practice with effective and proven processes.
By: Sue Zagula | On: October 12, 2018

In the blink of an eye Emergency Nursing 2018 came and went. The ENA conference is one of our favorite times of the year! It is an honor to have the opportunity to meet so many new nurses and catch up with familiar faces. Everyone at the conference is eager to uncover the latest in technology, education and research.
By: Sue Zagula | On: September 5, 2018

Gebauer’s Ethyl Chloride® topical anesthetic skin refrigerant has been trusted by healthcare professionals for more than 100 years. It’s possible you may not know the whole story about Ethyl Chloride, so we put together this QUICK FACTS guide.
By: Sue Zagula | On: December 19, 2017
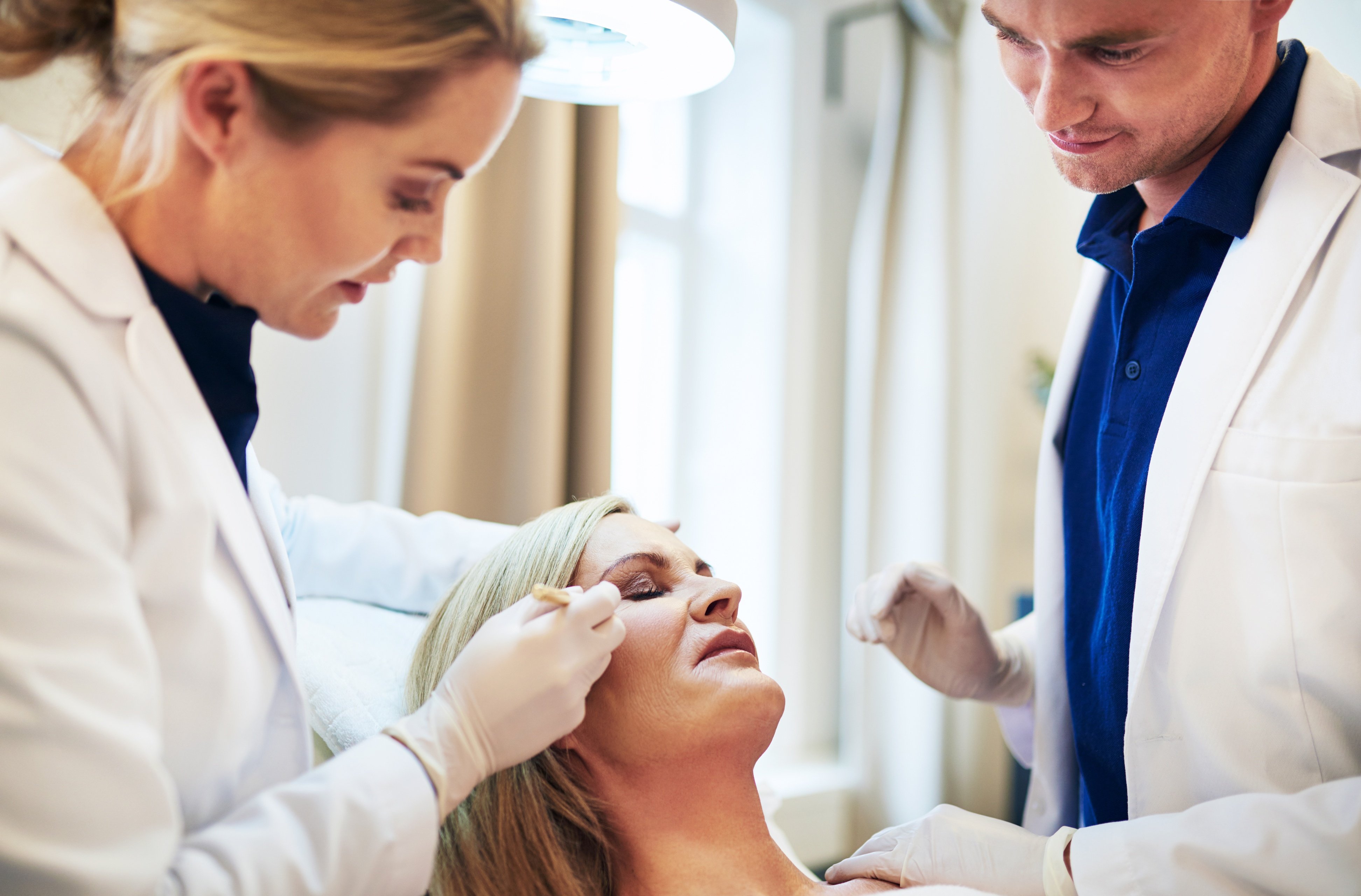
These days, people who need or want aesthetic treatments can shop around. Most feel any dermatologists can do Botox or fillers, so they will go to the one who’s offering the best deal. That’s why building patient loyalty is so important.
Outside of surgical revenue where fees are generally high, the most lucrative procedures are those where patients return for additional treatments. But practices lose patients all of the time— sometimes over very small price differences—when those same practices should be working to keep those same patients.
The good news is all of the elements that garner patient loyalty are simply good business practices. Although you may already may be doing some of them, you may need to put in a little more effort to make them work. Here are four things dermatologists can do to build patient loyalty.
By: Sue Zagula | On: December 14, 2017

When it comes to easing patient anxiety and improving the patient experience, the responsibility usually falls on you, the nursing professionals. Have you heard this question before: “Is this going to hurt?” Probably on a daily basis, right? But we found some time savers you can try that can get your patient the pain relief they’re looking for—faster.
You rarely hear a working nurse say, “Oh, I have plenty of time.” The fact is advances in medical technology are leading to a reduction in inpatient surgeries, but creating an increasing number of day-case procedures. This means you’re treating more patients each day and have limited time to spend easing patient anxiety.
The good news is that even in today’s fast-paced healthcare environment, nurses can provide patient comfort solutions in a matter of seconds, includingspray topical anesthetic. So, for you to quickly provide the pain relief your patients need, here are five time savers to help you provide patient care in the most efficient and caring way.
By: Sue Zagula | On: December 12, 2017
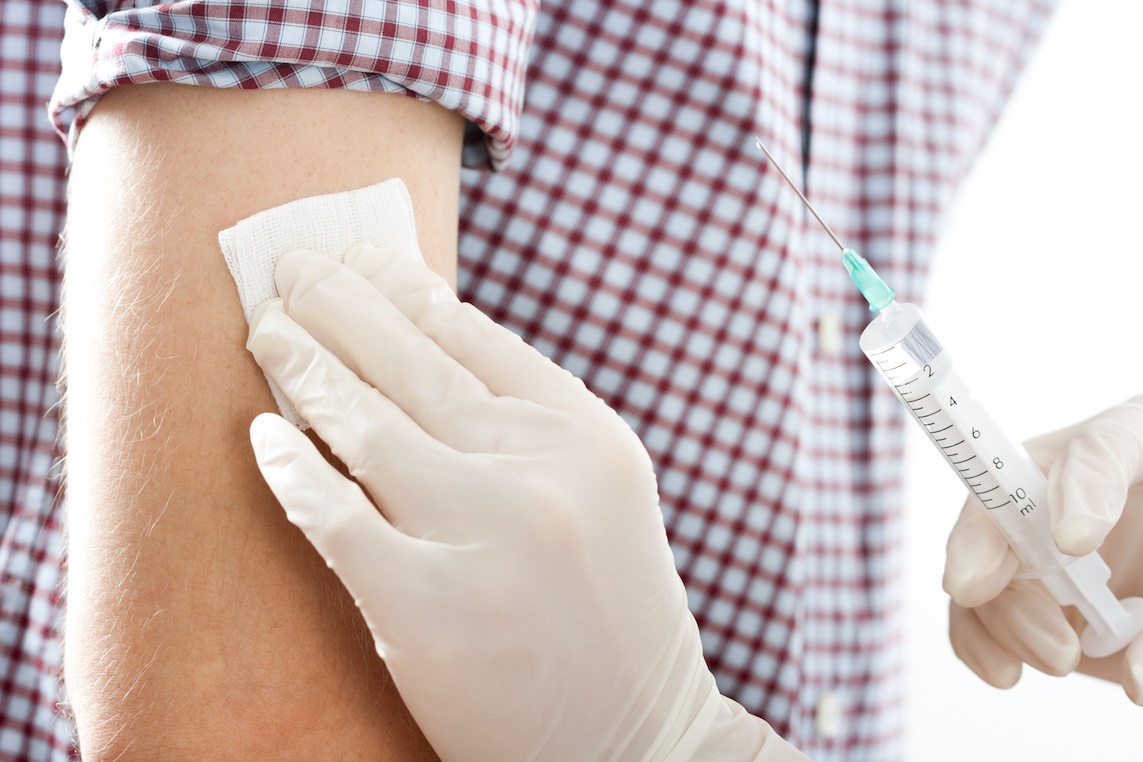
Flu season is here and no one knows that better than a nurse. You’re one of the first lines of defense in the fight against the flu. You may be called upon each year to administer flu shots to everyone 6 months and older.
According to the Centers for Disease Control and Prevention seasonal flu activity begins as early as October, can continue to occur as late as May, and commonly peaks in the United States between December and February. To help prevent transmission of the flu, many injections are given and with every injection comes a new person with different concerns.
Here are some reasons why nurses help fight the flu.
By: Jennifer Clark | On: October 3, 2017

A survey conducted by The Physicians Foundation found that nearly one-third of the physicians interviewed see up to 30 patients per day. If you take into account the average length of the face-to-face interaction between a physician and his or her patient in the exam room is 15 minutes, that doesn’t leave much time in the day to handle all of the other responsibilities that come with running a private practice.
The good news is there are several online tools for private practices than can help improve patient workflow and clinic efficiency while simultaneously providing a positive patient experience.
Here are six online tools clinicians should consider using.
By: Jennifer Clark | On: September 27, 2017

Are you considering furthering your education? Obtaining a bachelor’s or graduate degree can expand your earning potential and offer additional skills which can help improve the quality of care you administer.
Unfortunately, it may be difficult to find enough time to attend in-person local classes. Luckily, many colleges and universities offer online nursing degree programs.
Online nursing education offers a greater level of flexibility than on-site classes, but there are some potential drawbacks. Before you sign up for classes, you’ll want to consider these online program pros and cons.
By: Bethany Nock | On: September 21, 2017

While there’s no way to prevent 100 percent of mistakes in medical billing, healthcare organizations can still take some precautions to reduce the chances of a costly error.
In a previous article, we explored a few of the most common medical billing and coding issues. In this post, we’ll discuss how to identify potential risks of medical billing issues, how to resolve issues quickly when they do occur, and how to prevent the errors from happening again.
By: Sue Zagula | On: September 19, 2017

When a nurse actively pursues ways to expand his or her clinical knowledge and direct care skills, the benefits are twofold: 1) it can help stave off feelings of professional stagnation, and 2) it increases his or her value to the employer.
Seeking out opportunities for improvement can support better job security, boost your advancement potential and offer a general sense of accomplishment. Here are four ways you can stand out from the crowd and improve your nursing job security.
By: Bethany Nock | On: August 30, 2017
%20copy.jpg)
Nurses are often so busy in their daily job activities that other news in the nursing world such as new government policies and education requirements can often be pushed to the back of their minds. However, these things are important because they can affect all nurses. One way that nurses and nursing students can stay on top of changes in the field is by joining a professional nursing organization.
By: Bethany Nock | On: August 10, 2017

When your career is dedicated to improving the health of others, it can be easy to forget about your own health. However, in order to provide the highest quality care to your patients, you must take care of yourself, as well.
By: Jennifer Clark | On: August 2, 2017

Healthcare technology seems to be evolving at the speed of light. With changes happening so rapidly, healthcare organizations sometimes struggle to keep up.
By: Bethany Nock | On: July 27, 2017

There are two things nurses will never find excessive: vacation time and productive, efficient shifts.
By: Jennifer Clark | On: July 25, 2017

Technology always has had an impact on healthcare — from pacemakers and MRI machines to electronic health records (EHR) and robotics. The goal of these healthcare technologies has and will continue to be helping medical professionals provide the highest-quality, patient-centered care in the most efficient way possible.
By: Sue Zagula | On: July 19, 2017

Unfortunately, the push for instant gratification and a consumer-centric marketplace in retail and e-commerce now means people have unrealistic expectations in many areas of their lives — including health care.
By: Sue Zagula | On: July 13, 2017

No patient looks forward to a hospital stay, but while they are there, nurses have the greatest opportunity to make the visit a little more bearable.
By: Jennifer Clark | On: July 5, 2017

The healthcare landscape gets more competitive every day, which means marketing is no longer a “nice-to-have” for hospitals.
By: Jennifer Clark | On: June 28, 2017

Healthcare information technology enables clinics to gather and analyze an abundance of clinical and administrative data, but managing and using this information is challenging, especially without a reliable medical data management system.
Here is an introduction to medical data management systems and how they benefit physicians.
By: Bethany Nock | On: June 20, 2017

Anyone who has worked in a professional setting can tell you how important organizational culture can be. According to Forbes, “organizational culture is the collective result of how people on the team think and behave, their shared values and how they react to internal and external stimuli”. A cultural shift may be necessary when leadership is trying to implement change, such as increasing productivity or cutting costs.
By: Bethany Nock | On: June 14, 2017

Almost every parent has experienced the “we’re going to the doctor” meltdown at some point. Children often have fears associated with medical situations such as separation from their parent, anticipated pain, or simply fear of the unknown. This creates stress not only for the child, but also for the parent or guardian. Don’t worry, preparing your child beforehand can help make check-ups smoother.
Read through the four simple tips below to create a better experience the next time your child visits their physician’s office.
By: Sue Zagula | On: June 8, 2017

Are you considering going back to nursing school? You’re not alone. Twenty-nine percent of RNs plan to pursue a Bachelor of Science in Nursing (BSN) in the next five years, according to a study published in the Journal for Nurses in Professional Development.
Whether you’re interested in obtaining a BSN or an advanced degree, ask yourself these four questions before you sign up for classes.
By: Jennifer Clark | On: June 6, 2017

While the impact nurses and physicians have on the patient experience may be the most obvious, care providers are not the only members of the hospital staff who have the power to influence the patient experience.
Though a patient may never be introduced to them, hospital administrators still play a crucial role in what happens during a patient’s stay.
Here are three places where hospital admins have the greatest impact on the patient experience.
By: Bethany Nock | On: May 31, 2017

While every physician shares the primary responsibility of providing the best possible care to their patients, private practice physicians have the added challenge of running a business.
Managing a private practice can be expensive and exhausting, which is why physicians carefully choose their support staff — they want to make sure the clinic is filled with a team who can handle the administrative burdens so they can focus on patient care.
Once a physician has hired the best personnel for their clinic, the next step to ensuring the practice is run as efficiently as possible is to adopt a medical practice management system. A medical practice management system is a type of healthcare software that manages the day-to-day operations of a clinic, such as appointment scheduling, billing and other administrative tasks.
Here's what private practice physicians need to know about the basic components of a medical practice management system.
By: Sue Zagula | On: May 25, 2017

While a modern hospital may not have much in common with the locations where Florence Nightingale practiced, the mission remains the same: provide the highest quality of care in an environment focused on patient health and safety.
What can today’s nurses do to support this goal? Here are three ways staff nurses and nurse leaders can enhance hospital patient safety.
By: Bethany Nock | On: May 23, 2017

Though originally developed to deliver care to patients who had difficulty traveling to their primary care physician’s office, telemedicine services have evolved into an effective tool for providing convenient routine medical care for all patients.
As private practice physicians look for more ways to improve their clinic, offering telemedicine services is an effective option for increasing patient satisfaction as well as the profitability of the practice.
Here are three benefits of offering telemedicine services at your clinic.
By: Jennifer Clark | On: May 17, 2017

While the Affordable Care Act (ACA) has urged healthcare organizations across the country to change the ways they evaluate the care they provide, arguably the most important measurement the ACA highlighted is the concept of the “patient experience.”
Unfortunately, the best way to define the patient experience is up for debate, and every individual involved in a patient’s care has their own perception of which factors should be considered when assessing treatment quality.
However, among the most comprehensive investigations into the idea of patient experience was a 2014 article published in Patient Experience Journal, “Defining Patient Experience.” In this study, Wolf, et al. identified four distinct themes that practitioners—especially nurses—can use to help define and guide the patient experience.
Below is a discussion of these four elements.
By: Bethany Nock | On: May 11, 2017

How accurate are the claims submitted by your medical billing department? Given the complexities of the medical coding system, it’s not surprising that mistakes are made.
Unfortunately, even small errors can lead to claim denials and payment delays.
A March 2016 NBC News report noted an error rate of 7 percent to 75 percent in medical claims, depending on the source of the statistics. In 2010, the Office of the Inspector General reported that 42 percent of Medicare claims were improperly coded and 19 percent lacked sufficient documentation.
Whether the true error rate is closer to 7 or 75 percent, billing mistakes can have a big impact on your bottom line.
In addition to being costly for your hospital, these types of mistakes can also affect your relationship with patients. Avoiding common medical billing and coding mistakes will help reduce your error rate and keep your patients happy.
Here are five errors commonly made by hospital medical billers.
By: Jennifer Clark | On: May 9, 2017

Though nurses have a laundry list of responsibilities during each shift, when it comes to patient care, there are two main priorities: providing compassionate medical treatment and involving patients in care decisions.
Once these primary duties are addressed, most nurses choose to go above and beyond to ensure a patient’s stay at the hospital is as comfortable as possible. While there are dozens of ways to accomplish this goal, there may be a few you might not have considered.
Take a look at three uncommon ways nurses can improve patient care and increase satisfaction.
By: Bethany Nock | On: May 3, 2017

From organizing regular meetings between departments to scheduling procedures throughout the week, there are dozens of ways hospital admins can increase efficiency.
Regardless of the industry, it can be tempting to maintain the same processes that have been in place for years, but just as the healthcare industry is constantly evolving so too must a hospital administrator’s approach to managing their facility.
Here are three cutting-edge ways hospital admins can improve healthcare efficiency.
By: Jennifer Clark | On: April 27, 2017

Did you know that one of the first recorded reference to the nursing profession is on a pillar in India built around 250 B.C.?
Or that around the turn of the last century nurses worked, on average, 56 hours per week?
You don’t have to go back hundreds or thousands of years to hear some fascinating facts, however. Here are 10 thought-provoking statistics about modern nursing.
By: Bethany Nock | On: April 25, 2017

New graduates are often eager to leave the world of classes and studying behind, and jump feet first into their career. With a significant number of the current nursing workforce reaching retirement age, projected at 1 million by 2025, hospitals are adding more recent grads to the employment pipeline just to keep up.
Finding ways to develop these novice nurses into the best practitioners they can be by advancing their professional development often falls on the administrators’ shoulders.
A Nurse Residency Program (NRP) is one option intended to make the leap from student to practicing nurse smoother for everyone by focusing on leadership, patient safety, and interdisciplinary care. Below we’ll explore why your hospital should consider implementing this type of program and what benefits can be expected.
By: Jennifer Clark | On: April 19, 2017

We all look forward to the small victories during a busy day—for example, when a conversation we were dreading goes well or when we take a new approach to a task and it’s even more successful than we’d hoped.
Due to the nature of their job, the small victories nurses look forward to tend to be a little more unique. Here are 10 little wins that can instantly make a nurse smile.
By: Bethany Nock | On: April 13, 2017

A private practice physician’s interaction with a patient during a clinic visit may only last 10 to 20 minutes, but for the patient, the encounter started weeks ago when they scheduled the appointment and will last long after they leave the office.
Along with the support of his or her clinical staff, it is the responsibility of the physician to do his or her best to make sure the patient feels respected and appreciated at every stage of the process.
Here are five ways private practice physicians can provide a consistently positive experience for their patients.
By: Jennifer Clark | On: April 11, 2017

No matter how involved and empathetic you are as a nurse leader, there probably are a few things that your staff members don’t feel comfortable sharing with you.
Unfortunately, without an honest dialogue, it’s impossible to make the changes that will improve their skills, satisfaction and engagement.
Take a look at a few things that your nurses may be reluctant to tell you.
By: Bethany Nock | On: April 5, 2017

It’s difficult enough to survive in the competitive healthcare marketplace, but if your hospital doesn’t use the most cutting-edge practices and the latest healthcare technology, it can be especially challenging.
A hospital’s willingness to embrace innovation influences not only the decision of a patient seeking care but also the decision of a physician pursuing a new position. Using technologically advanced clinical processes and medical devices are an effective way to improve the patient experience, attract high-caliber staff and ensure compliance with regulations.
Here are three healthcare technologies that can help your hospital thrive.
By: Bethany Nock | On: March 30, 2017

Though healthcare has recently shifted from fee-for-service (FFS) payment structures to a value-based care (VBC) model, efficiency and productivity are still primary concerns for every care provider.
Healthcare technology, inventory management and proper interdepartmental communication are all essential for a productive and efficient healthcare facility. However, a hospital's design can have also have a big effect on patient flow, patient care and the patient experience.
Below are three ways to improve hospital design for increased productivity and efficiency.
By: Bethany Nock | On: March 28, 2017

To be successful in their role, nurses have a long list of skills and traits they must possess. Yet some days it can feel as if they need one more: mind-reading.
Patients aren’t usually the best at communicating what they want. This is somewhat understandable, however, since it’s intimidating to be in any unfamiliar situation, let alone one as stressful as a hospital stay.
Wondering what patients want during their hospital stay? Here are three things patients want from nurses during their time in the hospital.
By: Jennifer Clark | On: March 23, 2017

The average full-time employee in America works 46.7 hours per week. But as healthcare workers know all too well, hospital hours are long and often include double shifts. What is the effect of these long hours on employee health? Research shows that overwork can lead to poor sleep, depression, and even serious health problems such as diabetes and heart disease.
Busy nurses often think about the needs of their patients before their own. Making an effort to include wellness activities can help alleviate some of the stress nurses experience, as well reduce health risks. What are the benefits of a wellness program? We’ll cover this topic along with 10 ideas you can try right now.
By: Bethany Nock | On: March 21, 2017

Arguably one of the most difficult parts of being a nurse is delivering bad news to patients and their families.
Whether you’re informing a patient of an unfavorable diagnosis or telling someone their loved one has passed away, the situation is emotionally draining and one nurses dread.
To help make the task a little easier, here are a few tips for breaking bad news.
By: Bethany Nock | On: March 16, 2017

Sometimes, the most challenging obstacle a physician can face is establishing a strong connection with their patient.
The benefits of a good physician-patient relationship are numerous—higher patient satisfaction, better diagnostic accuracy, increased compliance to treatment plans and improved outcomes, to name a few—but breaking down the barrier between clinicians and patients can be difficult.
Here are five ways physicians can build better patient relationships.
By: Bethany Nock | On: March 14, 2017

Above all else, a nurse’s first priority is to provide high-quality care to his or her patients.
What comes after that can be different for every nurse, but likely the most common secondary goal is to be as efficient and productive as possible. Each nurse has his or her own tried-and-true methods for increasing efficiency and productivity, but sometimes it can be a good idea to think outside the box.
Here are four unexpected ways to improve nursing productivity.
By: Jennifer Clark | On: March 8, 2017

From vehicle maintenance to computer programming, quality assurance is an essential part of any service profession. The healthcare industry is no different.
Because low HCAHPS scores and failure to provide meaningful clinical statistics are becoming increasingly tied to lower reimbursement levels, it’s crucial for every healthcare organization to develop a quality assurance process. A strong quality assurance program is the key to meeting patient expectations and initiating changes that improve patient comfort, clinical outcomes and patient satisfaction levels.
These four steps will help you develop an effective healthcare quality assurance program.
By: Bethany Nock | On: March 2, 2017

Nurse leaders historically have been underrepresented on hospital governing boards. Although most boards included at least a few doctors, it was unusual to see a nurse serve. Unfortunately, that meant the very people who had important experience and insights about patient care didn’t have a voice in the way the hospital was run.
Today, as hospital leaders realize the importance of creating a collaborative environment, nurses are gradually being added to hospital boards. Supporting this initiative is The Nurses on Board Coalition (NOBC). Founded in 2014, the NOBC represents two dozen national nursing and other organizations, including the American Nurses Association, American Academy of Nursing and AARP. Its mission is to increase awareness of the unique perspective nurses can offer and ensure at least 10,000 nurses are on corporate and health-related boards as well as panels and commissions by 2020.
Becoming a member of your hospital’s governing board is an excellent way to initiate positive changes that will benefit the entire hospital and improve patient care. Here are three reasons that you should consider joining a governing board.
By: Jennifer Clark | On: February 28, 2017

At the end of a busy week, professional development is probably the last thing on your mind. Unfortunately, if you don’t make time for this, you’ll be overlooking an excellent chance to enhance your nursing skills, advance your career and improve the quality of care you provide your patients.
Every professional — especially nurses — should have a strategy for career development. In the dynamic healthcare landscape, there are many new opportunities to grow as both a care provider and a person. With an established strategy in place, you can make sure you’re always ready to take the leap into something new.
Keep these three steps in mind when you create your nursing professional development strategy.
By: Bethany Nock | On: February 14, 2017

Grants, Medicare payments and private payor reimbursements may be enough to keep a hospital running, but substantial improvements to a hospital require financial assistance from outside donors.
Successfully soliciting contributions can be challenging; taking the wrong approach can have major consequences. However, a healthcare organization's facilities can benefit tremendously from well-executed fundraising programs.
Read on to learn nine of the best practices for hospital fundraising.
By: Jennifer Clark | On: February 8, 2017
.jpg)
The demand for primary care is increasing, largely due to the Affordable Care Act (ACA), which granted healthcare access to many who were previously uninsured or underinsured.
A study conducted by Association of American Medical Colleges projected the demand for physicians to increase by 11 percent to 17 percent between 2013 and 2025. While demand for this type of care is increasing, the current trend shows a shortage of primary care physicians.
What can private practices do to ensure they can continue to meet the needs of their patients? One way is to tap into the skills of nurse practitioners to help fill in these gaps.
The American Association of Nurse Practitioners reports that there are more than 222,000 nurse practitioners (NP) licensed in the U.S. NPs are considered advanced practice registered nurses (APRNs) which allows them to assess patients, make diagnoses and prescribe medication, with or without physician oversight dependent on location.
This article will explore the benefits these clinicians can bring to your practice and how they can help you meet the growing demand for care.
By: Bethany Nock | On: February 2, 2017

There has never been a more exciting time to be a nurse. Not only is the number of clinical technologies designed to help make nursing easier and improve patient care constantly increasing, but the opportunities for growth as a nurse are increasing as well.
The healthcare environment is dynamic, with medical breakthroughs emerging every day. To stay ahead of the game, nurses must stay up to date with the latest trends as well as potential future healthcare developments.
As 2017 begins, take a look at these three trends to get an idea of what the future of nursing will look like over the coming months.
By: Bethany Nock | On: January 31, 2017

Along with “eat better” and “exercise more,” “learn more about the Hospital Inpatient Prospective Payment System (IPPS) final rule” should definitely be on your list of 2017 resolutions.
Unraveling the complexities of the hospital IPPS final rule will be a hefty undertaking, but if you get started now, you’ll be ahead of the pack.
Here are a few of the key ways the IPPS final rule will affect hospitals.
By: Bethany Nock | On: January 25, 2017

To be a nurse is to be a selfless caregiver. From the moment a nurse walks into a hospital or clinic, their main priority is protecting the health and safety of their patients.
While ensuring the health and safety of patients is essential, nurses can’t ignore the importance of their own health and safety. Nurses not only experience the challenges of professionals who are on their feet all day (such as muscle strain and fatigue) but they also face a unique set of risks not usually found outside a hospital or clinic.
To reduce health risks, injury and illness, pay attention to these four safety issues that affect staff nurses.
By: Bethany Nock | On: January 17, 2017

The Affordable Care Act (ACA) has had a big impact on the healthcare landscape. The legislation has led the shift from volume-based care to value-based care and makes health and wellness services available to millions of Americans who were previously unable to secure insurance coverage.
Healthcare professionals are familiar with a great deal about the ACA, but certain provisions of the law are not as well-known. For instance, did you know that Medicare reimbursement for services provided by certified nurse midwives (CNM) has increased to 100 percent of the Physician Fee Schedule? This means CNMs now receive the same reimbursement as physicians for services covered by Medicare.
Read on to learn even more fascinating facts about the ACA.
By: Bethany Nock | On: January 11, 2017

Even the thought of a double shift at the hospital can be exhausting. And if it’s an unplanned double, it’s especially taxing since you haven’t had a chance to properly prepare.
While a double is definitely challenging, there are a few ways you can make them a little easier. Here are five ways nurses can get through double shifts.
By: Bethany Nock | On: January 5, 2017

Whether a child is taking a math test or playing in a championship or receiving treatment in a hospital, he or she is bound to be anxious.
Just as a teacher has study guides to help the student get ready for the test or a coach runs drills to help the athlete be confident for the game, healthcare providers (and parents) can help pediatric patients prepare for a hospital stay using medical play.
Medical play is a therapeutic approach that uses real and pretend medical equipment, stuffed animals and dolls to assist pediatric patients in understanding not only the hospital itself but also what is happening with their own bodies. It is focused on activities that both enable a child to respond effectively to difficult medical situations and also support the child’s normal development.
In this post, we’ll discuss the best ways to leverage medical play and the benefits it can provide to pediatric patients, their parents and healthcare professionals.
By: Bethany Nock | On: January 3, 2017

Nurses have always played an integral role in providing quality care. New legislation from the last five to six years has provided even more opportunities for nurses to have an important part of enacting change.
There’s never been a better time for nurses to take an active role in healthcare management and innovation because of the Affordable Care Act. As a nurse leader, you are uniquely positioned to shape healthcare reform efforts in your hospital.
Keep these four focus areas in mind as you manage healthcare reform at your organization.
By: Bethany Nock | On: December 28, 2016

In health care, even minor changes to everyday procedures—for example, updating clinic protocol to include the application of a topical anesthetic before a procedure—take time to get used to. Every member of a care team, from a staff nurse to a physician, must update the routine that they’ve possibly been following for years.
When a major change is introduced, such as the recent transition from fee-for-service (FFS) payment structures to a value-based care (VBC) model for all healthcare systems, it means unprecedented changes in how healthcare organizations are run.
Whether you’ve just entered private practice or your practice has been open for years, it’s understandable to feel overwhelmed by the new reimbursement process. Although the new system may be challenging, these strategies can help make the transition easier.
By: Jennifer Clark | On: December 13, 2016
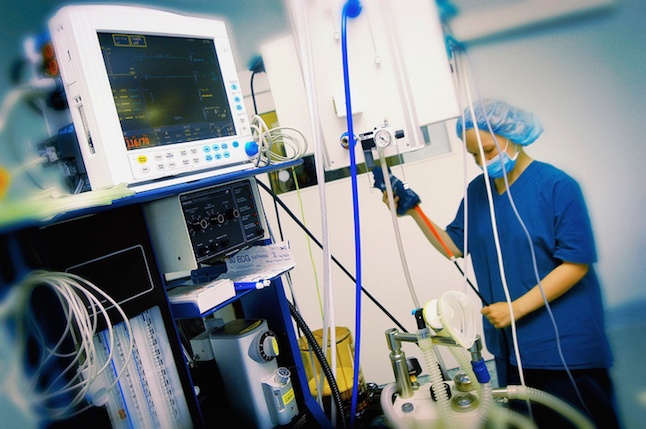
Technological innovations not only enhance patient-centered care but also help improve efficiency. Depending on the complexity of the medical device, the learning curve can be steep. If your staff isn’t thoroughly trained or lacks a basic understanding of the purpose and limitations of a machine or device, the risk of patient injuries increases.
Developing a comprehensive device training program can help you avoid these errors and ensure your patients receive the full benefits of the latest medical technology.
Keeping the following things in mind will help you develop an effective medical device training program.
By: Bethany Nock | On: December 7, 2016

Cost containment is one of the most important issues facing private practice physicians today. The price of supplies, increasing staffing costs and declining reimbursements all affect your bottom line, as does the constant need to update computer equipment and software. In fact, a 2016 Medical Group Management Association survey revealed that physicians spend $32,500 per year on healthcare technology alone.
Luckily, there are a few things you can do to tackle rising costs. These tips just may help you keep your costs down this year.
By: Bethany Nock | On: December 1, 2016

Hospital management teams are always on the lookout for methods to trim costs and improve efficiency. Since nurses account for a large percentage of the hospital staff, a frequently used strategy to decrease costs is to reduce the number of nurse labor hours. However, considering the Affordable Care Act (ACA) has placed greater emphasis on value-based care, the appropriate nurse-to-patient ratio is essential to guarantee patients receive the highest quality care.
Traditional nurse staffing systems fail to account for certain variables, resulting in staff shortages and an inability for nurses to spend adequate time caring for their patients. Newer staffing models are more flexible and can be adjusted to fit not only the needs of the entire hospital but also the needs of individual units.
Here are four approaches hospitals can take to ensure safe nurse-to-patient ratios.
By: Bethany Nock | On: November 29, 2016

Today, nurses are required to have, at minimum, an associate degree in nursing (ADN) to administer care. While every nurse has certainly received the clinical training required to provide quality care, having a Bachelor of Science in Nursing (BSN) usually leads to increased opportunities for personal and professional development.
Although there’s no doubt taking classes in addition to working full time will make life a little more chaotic, nurses who are interested in continuing their education should reflect on the advantages the degree can have for their patients, their hospital and themselves.
Here are three reasons why you should consider pursuing a Bachelor of Science in Nursing.
By: Bethany Nock | On: November 23, 2016

While the position of certified child life specialist is relatively new in the healthcare field, more and more hospitals are recognizing the positive impact child life specialists can have on patient satisfaction.
Every child life specialist performs certain duties—for example, providing emotional support to pediatric patients during their hospital stay and advocating on behalf of the patient in discussions with the healthcare team. But there are those child life specialists who go above and beyond to ensure their patients have the best possible hospital experience.
Here are three things the best child life specialists do every day to help pediatric patients feel more comfortable while they’re in the hospital.
By: Bethany Nock | On: November 22, 2016

Hospital stays aren’t something many people look forward to—you don’t get to sleep in your own bed, you have strangers coming into your room at all hours of the night and you have to spend all of your time in a hospital gown.
The one benefit of a hospital stay is that once it’s over, you usually feel a lot better than when you went in.
Many times an extended visit in the hospital is unexpected, but for patients who have the opportunity to prepare, here are five ways to make your hospital stay better.
By: Bethany Nock | On: November 10, 2016

Regardless of your industry or position, it can be easy to miss the forest for the trees. In medicine, that usually means viewing the procedure or the medication or the therapy as the totality of medical care. But patients perceive their experience holistically—from the first appointment to the final post-op evaluation.
Orthopedic surgeons who focus on the patient rather than their condition can provide more comprehensive, patient-centered care. They are adept at building personal, empathetic relationships with their patients, resulting in better communication and, in turn, increased patient satisfaction.
Read on to discover how to implement patient-centered care in orthopedics.
By: Bethany Nock | On: November 8, 2016
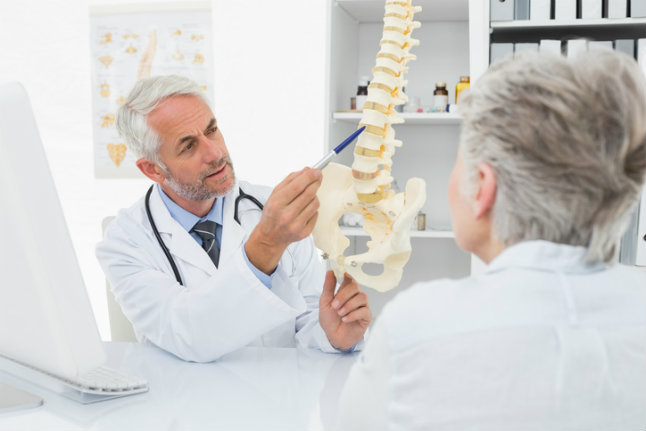
After four years in undergrad, orthopedic surgeons dedicate almost another decade of their lives to medical school and residency. When they’ve completed their residency, they’ve amassed a wealth of clinical knowledge to help them provide the highest quality care to their patients. However, in some instances there may not have been enough emphasis placed on an important aspect of care: patient communication.
Orthopedic surgeons are certainly skilled in the technical aspects of care, but some struggle seeing the patient experience as a whole, instead concentrating on the treatment. In this article, we’ll discuss some helpful tips orthopedic surgeons can use to improve their patient communication skills.
By: Bethany Nock | On: October 27, 2016

Here’s an interesting fact: In 2015 alone, the FDA approved nearly 70 new medications and over 40 new medical devices. Just five years ago, the number of medication and device approvals was 56, about half the 2015 total.
Because the sum of FDA approvals (and, in turn, the amount of clinical research trials) has surged in the last several years, there has been a dramatic increase in the need for qualified physicians to be a part of these trials.
While participating in clinical trials represents a significant time commitment, the benefits to medical institutions, patients and the physicians themselves are numerous. Here are nine reasons providers should consider participating in clinical research.
By: Bethany Nock | On: October 13, 2016

The benefits of community health programs are numerous. Improving the availability, accessibility and quality of healthcare in a particular area leads to a better quality of life for community residents.
However, developing health programs that effectively engage the community can be difficult for healthcare administrators. The goal of these initiatives is to meet the needs of the community, but it can be challenging just to identify those needs, let alone establish programs residents will actually use.
Read on to discover four ways healthcare administrators can improve community health planning and create a program that effectively promotes safety, healthy lifestyles, injury prevention and early detection of health conditions.
By: Bethany Nock | On: October 6, 2016

Providing the best hospital experience for patients requires coordination and communication between all providers involved in a patient’s care. This cooperative approach is referred to as interprofessional collaboration, and its goal is to help doctors and nurses work together to administer the highest quality care. Interprofessional collaboration fosters trust and respect between all healthcare providers and encourages the practice of treating nurses as equals with physicians.
In this post, we’ll discuss how nurses can collaborate across disciplines to ensure each healthcare professional’s expertise and experience are applied in the most effective way possible.
By: Bethany Nock | On: September 13, 2016
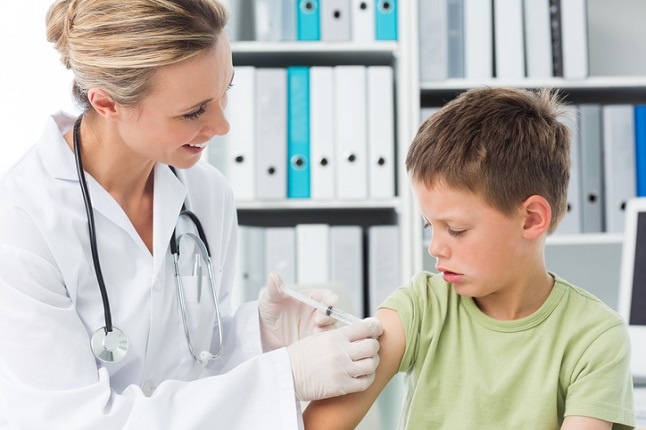
Along with buying art supplies and new outfits, immunizations can be an important part of the back-to-school checklist. It’s important for healthcare providers to keep in mind some valuable points when administering vaccines.
Below are three essential things healthcare professionals need to know about back-to-school immunizations.
By: Bethany Nock | On: September 7, 2016

Do too many of your new hires only last a year or two? High turnover not only strains your resources but can also affect quality of care. With just a few changes to your hiring, training and retention procedures, you can maintain (and boost) employee morale as well as improve patient satisfaction.
Here are a few hospital recruitment tips to help you attract and keep the most qualified employees.
By: Bethany Nock | On: September 1, 2016

It takes remarkable resolve to become a nurse and extraordinary determination to become a nurse leader. Taking the next step and transforming into a superior nurse leader requires an impressive level of commitment.
Great nurse leaders are experts in multiple areas: people management, administration and, of course, patient care. What makes a truly exceptional nurse leader? Here are five qualities all outstanding nurse leaders have.
By: Bethany Nock | On: August 30, 2016

We’re likely all familiar with the saying, “A chain is only as strong as its weakest link.” One of the reasons a nurse is promoted to the position of nurse leader is because he or she knows how to strengthen each link in the chain and help every member of his or her team reach their full potential. When a team is running at full capacity and has the support of the nurse leader, they can focus on administering the best quality care to their patients.
View the SlideShare below to learn seven ways nurse leaders can empower their team to provide patient-centered care.
By: Bethany Nock | On: August 24, 2016
When supervisors at hospitals and healthcare facilities are interviewing candidates, their primary concern is whether or not the prospective employee has the requisite clinical skills. While this is a crucial aspect of the hiring process, it’s equally important to evaluate soft skills, such as how a candidate works with a team, his or her communication skills and ability to collaborate.
Hiring a nurse who doesn’t fit within your organization’s culture can quickly disrupt the stability of your team and the efficiency of your organization. Here are a few tips to keep in mind the next time you conduct a nursing interview.
By: Bethany Nock | On: August 18, 2016

If you peer into the back of the supply closet of most private practices, you’ll find a stash of rarely used medical supplies. Maybe your staff ordered more tongue dispensers than you could need in a lifetime, or an “amazing new product” didn’t turn out to be so amazing after all.
Making poor supply choices not only hurts your bottom line, but it can also affect patient satisfaction—for example, if you run out of an important patient comfort product, it can negatively impact the patient experience. Keep the tips below in mind when you decide which products to keep or remove from your practice.
By: Bethany Nock | On: August 16, 2016

What would you say makes a good hospital administrator? Some attributes are obvious—for example, strong communicator, team player and effective negotiator.
Exceptional hospital administrators, however, possess a set of more advanced characteristics on top of these basic qualifications. These qualities help them ensure their organization is running as efficiently as possible and patients are completely satisfied with their hospital experience.
Here are four important traits every successful hospital administrator should have.
By: Bethany Nock | On: August 10, 2016

The Affordable Care Act (ACA) and the introduction of ICD-10 have complicated the already complex medical billing system. Due to changes in Medicaid and Medicare reimbursement as well as the different requirements for high deductible insurance plans, it’s becoming increasingly difficult for physicians to meet the financial goals they’ve set for their practice.
However, making the changes below may help improve the financial health of your practice and reduce the impact of the ACA.
By: Bethany Nock | On: August 4, 2016

With the introduction of the Medicare Electronic Health Record (EHR) incentive program and Meaningful Use, physicians have faced even greater pressure to balance efficiency and patient satisfaction. It can be difficult to input patient data accurately while simultaneously ensuring patients feel their concerns are being properly addressed.
The utilization of a medical scribe program can help doctors focus on providing a positive experience for their patients because the responsibilities of recording the patient’s past medical history and current complaints are delegated to a trained professional.
This post will examine the relatively new role of the medical scribe, including their training, primary duties and benefits to providers.
By: Bethany Nock | On: August 2, 2016

Auditing medical records can be a time-consuming process, but the benefits far outweigh the inconvenience.
In the simplest terms, a medical records audit is a chart review which is used to identify what is being done correctly and what is in need of improvement. Depending on the objective, medical record audits can be performed either by an external agency or by staff within an organization. Audits conducted by a third party are generally to review compliance, and internal audits are usually performed to evaluate current treatment processes and measure quality of care. This post will cover the latter.
Below is an eight-step guide on auditing medical records which nurses can use to ensure their facility is providing the best patient experience.
By: Bethany Nock | On: July 27, 2016

Many pediatric trauma patients are terrified when they arrive at the hospital. Fears about the extent of their injuries and concerns about their family members can make the experience even more overwhelming.
When children are too upset to respond to questions about their injuries, it can be difficult to know exactly how to treat them. Nurses who act as supportive advocates for their pediatric patients can help children cope with a potentially life-changing event and minimize emotional trauma.
Here are four ways nurses can improve the hospital experience for pediatric trauma patients.
By: Bethany Nock | On: July 21, 2016

Living with a chronic illness is difficult no matter your age, but it can be particularly hard for pediatric patients. Without appropriate coping skills, they may fail to comply with their treatment plan (either deliberately or unintentionally), which can result in more frequent hospitalizations and avoidable complications.
Here are a few ways your nursing staff can help pediatric patients cope with chronic illness.
By: Bethany Nock | On: July 13, 2016

Whether you’ve recently graduated with your BSN, or you’ve already spent a few years at a hospital and are looking for something new, many different roles in the field of nursing can be the next step in your career.
In this article, we’ll discuss four career paths in the nursing field you can take if the clinic or hospital environment is not the right fit for your professional goals.
By: Jennifer Clark | On: July 7, 2016

Nurses typically have the most contact with patients, meaning they are likely in the best position to be their voice in discussions about their plan of care with doctors, support staff and even family members.
The core ideology of patient advocacy is ensuring the patient’s satisfaction and safety, while advocating for their best interest. Here are four tips you can use to be strong patient advocates.
By: Bethany Nock | On: July 5, 2016

Unclear or inadequate communication is frustrating, but communication breakdowns can be downright dangerous when it comes to patient care.
In large hospitals and medical centers where information is exchanged between multiple departments, there is an even greater risk that crucial details won’t reach the right person in a timely manner. Unfortunately, this can lead to poor outcomes and even death.
By: Bethany Nock | On: June 23, 2016

A violation of HIPAA regulations, even if the infraction is accidental, can be costly.
If HIPAA rules are unintentionally violated, the Office for Civil Rights assesses a $100 fine per offense. If the infraction was willful and no attempt was made to correct the problem, the fine can escalate to $50,000.
HIPAA violations can cost your institution thousands of dollars and damage the relationships you’ve worked so hard to establish with your patients. These tips can help you ensure HIPAA compliance and keep patient information safe.
By: Bethany Nock | On: June 21, 2016

In this era of patient-centered care, motivating patients to take charge of their health care is more important than ever. Patients who take a more active role in managing their health are more likely to stick to treatment plans and often experience an improved quality of life.
This five-step guide will help you how to promote patient independence and teach patients how to become more autonomous.
By: Bethany Nock | On: June 15, 2016
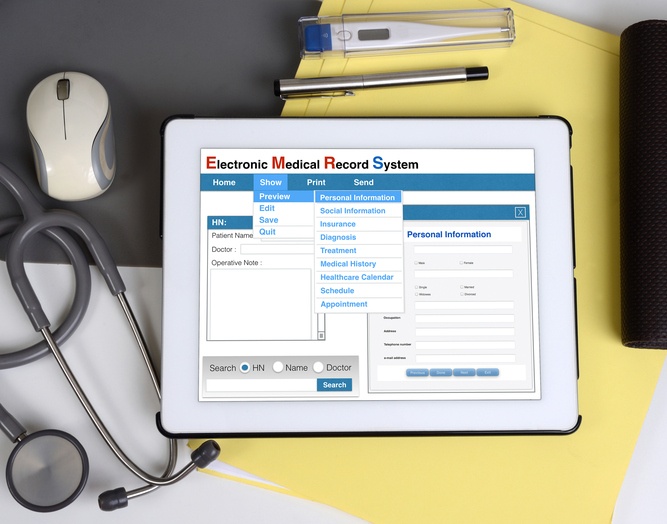
The Medicare Electronic Health Record (EHR) incentive program and Meaningful Use have been controversial since their establishment in 2010. The popular opinion was they placed too much importance on patient data and not enough on the actual patients.
The good news is the Centers for Medicare and Medicaid Services (CMS) recognized the flaws in the system and announced in January 2016 that Meaningful Use as it currently existed would be discontinued.
Read on to learn what brought about this reform and how it could impact your practice.
By: Julianne Filion | On: June 8, 2016

Hospital visits and trips to the doctor’s office are rarely pleasant, and chronically ill pediatric patients (along with their families) must make those treks on an all-too-often basis. Healthcare professionals who sympathize with this and adopt patient-centered care tend to see higher levels of patient satisfaction since the focus is on providing the best possible experience for their patients.
In this article, we discuss three types of pediatric therapy that can help foster a more positive environment for your patients and their loved ones.
By: Julianne Filion | On: June 2, 2016

Although they’re following traditional American customer care best practices, your nursing staff may be unintentionally disrespectful to patients if they aren’t taking the patient’s cultural or religious background into account during interactions. Behaviors that are acceptable to some of your patients, such as shaking hands or making eye contact when speaking, may be seen in an entirely different way by patients from other cultures.
Emphasizing culturally congruent care—an approach that blends patient care with patient values, beliefs, lifestyle and traditions—can help every patient feel comfortable and increase your CAHPS scores. Culturally congruent care involves a personalized approach, rather than a cookie cutter method.
Avoiding the following errors will help you ensure patients are satisfied with the care they receive.
By: Bethany Nock | On: May 26, 2016

As a hospital administrator, you’re always looking for ways to improve workflow and increase patient comfort. For example, you may decide to revise the process for patient admission or perhaps add a new product to your hospital’s standard treatment regimen. However, sometimes products that look good on paper don’t always deliver the results you expect.
How can you avoid investing money in a product that may not be a good fit for your institution? Conduct a product pre-trial. These can also be called product evaluations, product assessments, product reviews, etc.
This post will cover why to conduct a product pre-trial, how to start the process and the steps involved in the trial.
By: Julianne Filion | On: May 24, 2016

Are you a nurse who’s passionate about improving the quality of care your patients receive at every stage of their visit, from check-in to discharge?
Are you ready to step into a leadership role and coach staff members on the practices that would benefit your patients and your institution?
Can you coordinate communications within your own department and across departments?
If you answered yes to these questions, then you just might have what it takes to be a successful nurse leader. Take our quick quiz to find out if you are ready for the next step in your nursing career.
By: Julianne Filion | On: May 18, 2016

You’ve worked hard to improve the culture of your hospital and are finally seeing the fruits of your labor with improved HCAHPS scores, reduced turnover and increased employee satisfaction. Unfortunately, it only takes a few incidents of lateral violence among your nursing staff to undo your efforts.
In the past, lateral violence was largely ignored. “Nurses eat their young,” was the joke, and it seemed no one cared to change the status quo. While today’s environment is better for both patients and hospital employees, this doesn’t mean lateral violence and bullying are no longer an issue. As a nurse leader, it’s up to you to creating a plan to change attitudes and behaviors, and finally putting an end to the problem.
By: Julianne Filion | On: May 12, 2016
 If you’re like most nurse managers, preparing the nursing department annual budget is not your favorite part of the job. The budgeting process can make even normally calm, collected nurse managers resort to a few choice words as they struggle to create a budget that won’t shortchange patients and nursing staff.
If you’re like most nurse managers, preparing the nursing department annual budget is not your favorite part of the job. The budgeting process can make even normally calm, collected nurse managers resort to a few choice words as they struggle to create a budget that won’t shortchange patients and nursing staff.
These days, “budget cuts” is a common phrase among hospital administrators. Although running a lean organization is essential to the survival of your hospital, when cuts affect crucial services, it can be difficult to reconcile your facility’s mission to provide excellent care with cuts that surely will affect the quality of patient-centered care.
By: Julianne Filion | On: May 9, 2016

May is National Nurses Month, an annual opportunity to show nurses appreciation for the outstanding contributions they make to your community.
Nurses wear quite a few hats: confidante, advocate, adviser, counselor and, of course, caregiver. We should always do our best to remember just how important nurses are.
By: Julianne Filion | On: May 4, 2016

Long shifts, varying work styles and power struggles can contribute to dissension among your nursing staff. Patient satisfaction and engagement, as well as productivity and attention to detail suffer when team squabbles occur. This can, unfortunately, affect your HCAHPS scores. Of course, building a cohesive team takes time, but it’s well worth the effort. Here are a few ways you can help your nursing staff develop stronger relationships while creating a cohesive team environment.
By: Julianne Filion | On: April 28, 2016

The emergency department is without question the most dangerous place in the hospital for nurses. Combative patients, upset families and personal confrontations that spill into the emergency room can make the ED environment volatile at times. While you’re treating the AMI patient or juggling an influx of patients from a multi-car accident, the last thing you should be concerned about is your personal safety. That’s why we put together these tips to help your hospital advance nursing staff safety in the emergency department.
By: Julianne Filion | On: April 20, 2016

Running a private practice is doubly hard when you’re a pediatrician. From crying, anxious children to nervous adults, not only do you have to keep your patients happy, but you also have to make sure parents are satisfied, too.
The best pediatricians have found ways to improve pediatric patient experiences using easy-to-implement tactics. Here are a few strategies you can use to support both your patients and their families.
By: Julianne Filion | On: April 14, 2016

The transition from pediatric to adult care can be confusing for patients, parents and families. It means new doctors, new routines and possibly new treatment plans. Furthermore, the transfer of legal responsibility to the patient (upon reaching adult age) can be emotionally and logistically troubling for parents or caregivers. This doesn’t even take into account the numerous life changes these young adult patients are already facing outside their medical care.
Transitioning pediatric patients shouldn’t be taken lightly, as many unforeseeable challenges could deter patients from receiving the care and support they require and deserve. But sadly, more than 50 percent of parents polled by the National Survey of Children with Special Health Care Needs claimed no one even spoke to them about the upcoming need for their child to switch to adult care.
By: Julianne Filion | On: April 12, 2016

Hospitals have a way of making children feel vulnerable and afraid, especially when their visit involves surgery. Any time a child requires surgery, parents understandably get emotional. Fear, worry, stress, anxiety—these are all powerful reactions to pediatric medical procedures that healthcare professionals must handle with compassion.
Instinctively, healthcare professionals focus on physical health first. But mental health is scientifically proven to have a significant impact on physical wellbeing, which means it must also be a medical priority. Pediatric patients are particularly difficult to care for in this realm because sometimes they struggle to express how they’re feeling or advocate for what they want or need.
That’s where exceptional communication becomes a critical part of care. In most cases, it is the uncertainty about a surgical procedure that amplifies a pediatric patient’s emotions (and consequently, their parents’). With the right approach and communication skills, healthcare professionals can help younger patients feel less vulnerable and more included in their own treatment plan. Follow these tips on how to communicate with pediatric patients before surgery to make their hospital stay less traumatic.
By: Bethany Nock | On: March 31, 2016

You know that frustrating feeling when you are looking for a gauze pad, but you can’t find it? And it turns out you can’t find it because it is listed under New Gauze or the manufacturer of the product on your inventory list? (We can almost see you nodding your head right now.) All you want to do is take care of your patient, but inventory management is making it difficult.
Maintaining supplies may be an essential part of your job as a nurse leader, but we understand it can be hard to keep up with inventory management (or influence it when you don’t control it) when you have so many other responsibilities.
Developing a strong relationship with the materials management department, taking advantage of the capabilities of digital inventory control and using a few old-fashioned tips can help you stay on top of this portion of your job, even on the craziest of days.
Here are a few tips to help nursing inventory supply and to ensure your staff is never without the supplies it needs.
By: Julianne Filion | On: March 29, 2016

Your shift starts off with one of your patients crashing, your new admission arriving, and the gentleman in room 204 falling and hurting himself. Immediately you feel the pressure of all you have to accomplish. You may be thinking, “How will I get this all charted in a timely manner and still handle my med pass on time?” The healthcare industry has recognized this plight and has made strides to help nurses more efficiently handle their daily tasks, including charting.
By: Bethany Nock | On: March 16, 2016

With patient satisfaction ratings tied to reimbursement levels, it’s more important than ever to ensure patients have a positive experience at your hospital. A pet therapy program offers a low-cost, low-tech way to improve the patient experience without impacting staffing levels. Not sure if a pet therapy program is right for your hospital? Consider these benefits before you make your decision.
By: Julianne Filion | On: March 10, 2016

Most of us do it—if not for ourselves, for someone we care about. We Google symptoms and self-diagnose before we decide whether or not to see a physician. In fact, Pew reports that 72 percent of Internet users search for health-related information online.
Think about it: how many times have you arrived for a doctor appointment prepared with a list of possible reasons for your ailment?
By: Julianne Filion | On: March 8, 2016
 Family members play an important role in a patient’s recovery. They’re often the ones who make sure their loved one takes medications, makes necessary lifestyle changes and follows aftercare recommendations. Although family members can provide the support recovering patients need, sometimes they become overly involved in the decision-making process.
Family members play an important role in a patient’s recovery. They’re often the ones who make sure their loved one takes medications, makes necessary lifestyle changes and follows aftercare recommendations. Although family members can provide the support recovering patients need, sometimes they become overly involved in the decision-making process.
When relatives try to control a patient, rather than support him or her, trouble lies ahead. All too often, hospital staff members become caught in the middle. It’s crucial for family members to understand how they can provide a supportive role.
Striking the right balance isn’t always easy, but as a medical professional, you can help educate family members about helpful roles they could take on using the following talking points.
By: Bethany Nock | On: March 2, 2016
 Attracting new patients is a constant concern for most physicians in private practice. Whether you want to expand your practice or just make sure your patient load remains stable, adding new patients is an essential aspect of your business. These three strategies will help you attract and keep quality new patients to grow your private practice.
Attracting new patients is a constant concern for most physicians in private practice. Whether you want to expand your practice or just make sure your patient load remains stable, adding new patients is an essential aspect of your business. These three strategies will help you attract and keep quality new patients to grow your private practice.
By: Bethany Nock | On: February 25, 2016
 It may be a cliché, but your employees really are your most valuable assets. If you fail to create a strong work culture, you risk losing your best employees to your competitors. The entire hospital suffers when your top performers decide there are better places to work. Without the best and brightest, it’s difficult to create a positive culture that not only empowers and engages employees but also improves the patient experience.
It may be a cliché, but your employees really are your most valuable assets. If you fail to create a strong work culture, you risk losing your best employees to your competitors. The entire hospital suffers when your top performers decide there are better places to work. Without the best and brightest, it’s difficult to create a positive culture that not only empowers and engages employees but also improves the patient experience.
Here are steps healthcare administrators can take to ensure a positive work atmosphere for employees.
By: Julianne Filion | On: February 23, 2016

For nurses with ever-changing schedules, adapting to changing shift cycles can present several unique challenges. Shift work isn’t always kind to your circadian rhythm—the body’s natural clock that keeps us awake during the day and slows us down at night.
Patient care is a 24-hour operation, so to take care of yourself and ensure patient safety and satisfaction, it’s necessary to make adjustments to your sleep schedule and daily routine. Especially for busy nurses who are always on their feet, self-care is crucial for job satisfaction and improving the patience experience.
To provide the best nursing care and remain focused and productive, here are three tips to stay healthy and well rested despite a shifting schedule:
By: Bethany Nock | On: February 17, 2016

Complicated paperwork, lengthy waits and concerns about your condition can increase your stress level when you visit the doctor. By the time your physician asks if you have any questions, you may feel so overwhelmed that you forget to ask about important issues. Preparing a list of healthcare questions in advance, including those listed below, will help you make the most of your time with the doctor and increase satisfaction with your experience.
By: Bethany Nock | On: February 11, 2016

Keeping your youngest patients happy can pose a significant challenge for you and your staff. No matter how welcoming your pediatrics unit may be, it’s just not home. Anxiety about medical procedures, coupled with the unfamiliar sights and sounds of a busy hospital, can lead to an unpleasant experience for some children. Nurses and other staff members can’t always spend as much time as they would like calming scared or anxious children, but certified child life specialists can fill the gap.
Although child life specialists have long been employed at children’s hospitals, administrators of other healthcare facilities are now realizing the value of hiring these specialists.
By: Julianne Filion | On: February 9, 2016

Nurses play a critical role in caring for patients and improving outcomes, but also ensuring hospitals maintain higher HCAHPS scores. While some staff changes are expected, a high turnover rate can be disruptive to the team and affect patient care and satisfaction. As a nurse leader, it can be frustrating to train and manage a nurse only to have him or her become unengaged, or worse, leave the job. So what can you do to change the trend?
Nurse leaders can help reduce turnover. But, first, let’s look at what leads to turnover.
By: Bethany Nock | On: February 3, 2016

When your entire job centers on caring for others, it’s easy to let your own health and wellness fall by the wayside—especially when it comes to maintaining a work-life balance. Overseeing a practice means managing a staff and business finances, providing services to your patients and keeping them fully satisfied. Given everything on your shoulders, it’s easy to fall into the habit of working long hours with little or no break. However, burnout can (and will) eventually rear its ugly head.
There’s a common misconception in the medical field that to be successful, you must make extreme personal sacrifices. While getting to where you are certainly required a great deal of discipline and dedication, it doesn’t mean you have to give up the idea of a balanced life.
Here are a few tips to help you achieve harmony in work and life while still meeting goals for your practice.
By: Bethany Nock | On: January 28, 2016

Ahh, New Year’s resolutions. Everyone begins the year so committed, so hopeful and so diligent. According to Nielsen, the two most popular resolutions in the United States are “staying fit and healthy” and “losing weight.” As a physician, that’s likely music to your ears.
Now for the not-so-great news: Research also says 25 percent of people who make health resolutions can’t even make it through the first two weeks. Given that we’re already nearly a month into the new year, 1 in 4 have likely already thrown in the towel.
Luckily, there’s still time to get your patients back on track and committed to preventive care in 2016. Here are a few ways you can increase their success rate.
By: Bethany Nock | On: January 26, 2016

Thanks to unlimited access to healthcare information online, today’s patients are more informed than ever before. With a few strokes of a keyboard, anyone can search their symptoms and instantly access page upon page of health and wellness advice. Unfortunately, this proliferation of health resources also leads to an increase in the opportunity for misinformation and incorrect self-diagnosis.
Misinformed patients can be a patient communication challenge for healthcare teams. Luckily, because nurse leaders and their staff are frequently the first to interact with patients and their families, they can immediately start the process of clearing up misconceptions and help increase the likelihood of better outcomes.
Here are four tips to foster better communication with misinformed patients, quell unnecessary anxiety and ensure improved patient comfort and satisfaction.
By: Bethany Nock | On: January 21, 2016

Can you believe we’re already three weeks into 2016? Like many business owners, you likely spent the beginning of the year reflecting on previous successes and setting new goals. What are you doing to ensure your practice continues to be successful this year? To help you get on the right track, we’ve put together a list of five private practice goals you should focus on to help you improve and strengthen your practice in the coming year.
By: Bethany Nock | On: January 19, 2016

It’s difficult to commit to a patient-centered care approach without input from patients. Although surveys are helpful, they’re no substitute for conversations with people who’ve been patients in your hospital. If you want to make sure you’re providing the services your patients truly need and want, the best course of action is to create a patient advisory board.
We’ll take a look at the many benefits of developing a patient advisory board, and how you can get started.
By: Bethany Nock | On: January 14, 2016

Have any of your patients complained about wait time? Have any of your staff members become frustrated by inefficiencies in the appointment process? Have you ever felt burned out and unable to keep up with patient flow? If you answered yes to any of these questions, you’re not alone. Even the most successful private practices are challenged by creating, optimizing and maintaining processes for managing patient flow.
By: Bethany Nock | On: January 12, 2016

Evidence-based care helps you make the best treatment decisions and it can revolutionize your practice. Although the care model involves consulting the latest research studies for information about treatment benefits and protocols, it’s about more than simply relying on research studies to make decisions. Your personal experience and input from your patients are also important considerations.
By: Bethany Nock | On: December 15, 2015

For years, your hospital has been dedicated to offering the best possible care to each and every patient. Your staff members are unwavering in their commitment to integrate the most innovative medical advances, and apply their ample knowledge and experience to develop sustainable care plans. While your hospital is devoted to helping each patient thrive, you may still be missing one piece of the patient satisfaction puzzle: patient engagement.
By: Julianne Filion | On: December 9, 2015

Only 66 to 76 percent of hospital patients feel that their pain is well-controlled, according to the latest Summary of HCAPHS Survey Results. Poor pain management can contribute to a variety of problems, including longer hospital stays, delayed wound healing, chronic pain syndrome, depression and substance abuse.
By: Bethany Nock | On: December 3, 2015

Bottlenecks caused by patient flow not only reduce efficiency and revenue, but also affect patient satisfaction levels. Improving flow starts with evaluating current systems and procedures to determine whether they are effective or are just hampering your efforts to provide quality healthcare.
By: Julianne Filion | On: December 1, 2015

It’s near the end of an exhausting shift. You’ve finally assigned each patient to a member of your staff, and you’re just sitting down to begin your charting. As you open a file, you begin to daydream about the fuzzy slippers and hot cup of tea you’ll soon enjoy at home. It’s been a long day but, unfortunately, it’s about to get even longer.
By: Bethany Nock | On: November 25, 2015

When it comes to healthcare’s pay-for-performance model, hospitals aren’t the only ones feeling the effects. Today, under the Affordable Care Act, physicians are expected to participate in the Physician Quality Reporting System (PQRS) — or begin facing penalties as early as next year. Private insurers also are adopting value-based payment.
By: Julianne Filion | On: November 24, 2015

Difficult patients have one thing in common: they are unhappy with some aspect of the service they’ve received at your facility. Whether a complaint is justified or it feels like the patient is being completely unreasonable, your responsibility is to address the complaint diplomatically and ensure it will not negatively affect the patient’s satisfaction.
By: Bethany Nock | On: November 18, 2015

Technology is always changing, and staying on trend can take more time and effort than you have available. When it’s time to invest in healthcare technology for your facility, how do you know which products will improve the patient experience and save money, and which are unnecessary and overpriced?
From a new EHR to an upgraded network, data storage to phone systems, you need investments that will yield the best returns — whether monetary or in the form of increased efficiency. Keeping the following things in mind will help you spend your money wisely.
By: Bethany Nock | On: November 12, 2015

In the last few decades, the healthcare industry has experienced rapid technology growth and evolution. These advancements have led to more effective treatments, increased patient comfort and better outcomes overall. The technology boom also means more providers in the market — which means the decision-making process isn’t always easy.
As a healthcare administrator, you know even the smallest of choices can make a significant and lasting impact on your facility and the patients you serve. So when it comes to choosing medical device providers, you want to ensure you’re fairly assessing all options.
In an effort to help ease the decision process, we’ve created a list of the top 4 questions to ask when comparing medical devices and medical device manufacturers.
By: Julianne Filion | On: November 10, 2015

Have you ever felt like you were living in a fog? Even with plenty of rest, you still felt physically and emotionally exhausted. Maybe you found yourself hitting the snooze button a few more times than usual, struggling to maintain focus throughout the day and perhaps even snapped at a coworker or two. Even though you love being a nurse, you might have felt overwhelmed and unenthused.
Although these experiences seem commonplace to any hardworking professional, they’re actually the telltale symptoms of a much larger issue. Burnout is a real (and frustrating) condition, and the additional stressors placed on those in the nursing industry put professionals like you at a higher risk for burnout than workers in other professions.
If you’re beginning to feel the onset of burnout, follow these five tips to a healthier, happier and more fulfilled you.
By: Bethany Nock | On: November 4, 2015

Physicians know preventive care is effective in reducing the likelihood of heart disease, diabetes, cancer and other common diseases. But convincing your patients that the result is worth the changes in lifestyle can be a struggle. Concern about costs and lack of knowledge about the benefits of preventive care are the leading contributors to patient apathy.
The good news is there are a few things you can do to encourage your patients to embrace prevention as a long-term strategy for better health.
By: Bethany Nock | On: October 29, 2015

Long waits, harsh lighting, loud noises and a sense of powerlessness can make a hospital visit confusing and uncomfortable for both parents and their children. The following tips can help you ensure your young patients, and their parents, have a positive experience while visiting your facility.
By: Julianne Filion | On: October 27, 2015

When patient needs and concerns are held in high regard, everyone in your facility benefits. But making the switch to a patient-centered culture isn’t always easy. Your team may oppose change and see these revisions as yet another task on their already long to-do lists.
Achieving buy-in is the foundation of supporting a culture of patient-centeredness within your hospital. As a nurse leader, it’s up to you to be a catalyst for culture change. By modeling appropriate behavior and guiding your staff as they adapt to new standards and expectations, you can help everyone successfully adopt this culture shift.
Here are some tips for creating more patient-centeredness in your workplace:
By: Bethany Nock | On: October 21, 2015

When you’re craving sushi on vacation, Yelp can help you find the highest rated Japanese restaurant in town. If your roof is leaking, you can consult Angie’s List to find the best reviewed local contractor. But what do you do when you need to schedule surgery, make a late-night trip to the ER or find the best labor and delivery department for your child’s birth? How can you adequately, and conveniently, assess healthcare organizations to find the best hospital for your specific needs?
To help you do the right research and choose the prime facility for your healthcare needs, we’ve compiled a list of the top three questions to consider when choosing a hospital:
By: Julianne Filion | On: October 13, 2015

Remember your first day at your first nursing job? For at least two years you endured a grueling schedule of nursing school courses and early morning clinicals, survived graduation and passed your NCLEX with flying colors. By the time you obtained your first job offer, you were bursting with excitement and ready to jump head first into your new career. But, on the first day, you arrived a bundle of nerves. How could you make sure you consistently provided the best care and experience to your patients? Who would you turn to for guidance?
As a nurse leader, it’s likely been several years since your first day on the job. Through hard work and dedication, you achieved a leadership position. Although those early days of your career may now be nothing but a distant memory, it’s a current reality for several of your newer nursing team members.
To ensure patient satisfaction, and help your new staff members succeed, here are three tips for helping new nurses communicate better with patients:
By: Bethany Nock | On: October 7, 2015

Your job is growing in importance. From keeping up with ever-changing regulatory and compliance updates to managing patient satisfaction processes and overseeing staff, healthcare administrators like you fill an exceedingly demanding role. Not to mention, now you’re tasked with handling the electronic health records roll-out and other federally mandated updates. Given your full plate and maxed-out schedule, you need to know you can depend on the support of your team. In fact, it’s more important than ever to keep your team as efficient as possible.
Here are our top tips for increasing team efficiency and productivity without increasing your budget:
By: Julianne Filion | On: September 30, 2015

When a patient is admitted to your hospital, it’s up to you, your team and your hospital’s physicians to treat his or her concerns fully and completely. Theoretically, if you accomplish this task, your patients will start a successful road to recovery and return to their lives. Unfortunately, this isn’t always the case.
Unplanned hospital readmission, or a patient’s return to the hospital for the same or related issue is not only inconvenient for the patient, it also poses a significant concern for hospitals. That’s because, as of October 2012, the federal government began penalizing hospitals with excessive readmission rates in the form of reduced Medicare reimbursement. Not to mention, readmissions can affect patient satisfaction and strain hospital resources.
Because nurse leaders play such a vital role in a patient’s hospital experience, it’s often up to you and your team to reduce the risk of readmission. To help you achieve this goal, we’ve put together three tips to decrease your hospital’s unexpected readmissions:
By: Bethany Nock | On: September 24, 2015

Over the last several years, patients have begun taking a much greater vested interest in their health and wellness. While patients of previous generations took their doctor’s word at face value, today’s patients are researching their symptoms and conditions online, downloading case studies and engaging with other patients in internet forums. While this means some patients arrive for their visit armed with a self-diagnosis and droves of misinformation, it also means people are becoming more invested in their treatment.
To leverage this interest, and help patients take a more active role in their care plan, many healthcare providers are using Shared Decision Making (SDM). In other words, it’s a strategy in which, instead of making a decision on a patient’s behalf, clinicians provide patients with the knowledge they need and walk through the decision-making process together.
Here are three things you should know about SDM, and how to best implement it in your own practice:
By: Julianne Filion | On: September 22, 2015

Whether you’re brand new to your role or a seasoned pro, every leadership position comes with its share of challenges. Although improving management skills and team collaboration is important for leaders in any industry, for nurse leaders it can impact whether or not your hospital receives full Medicare reimbursement or your private practice maintains maximum efficiency.
At the end of the day, it’s up to you to ensure your team is working together to produce the best results for your institution, offering the best nursing care to each and every patient and experiencing job satisfaction. Consider the following five tips nurse leaders can use to improve team cooperation:
By: Bethany Nock | On: September 17, 2015

You’ve heard the old adage “one bad apple spoils the whole bunch.” When it comes to online reviews for private practice physicians, this couldn’t be more accurate. Despite the glowing opinions of your most loyal patients, a few unhappy respondents can drive down your score and leave prospective new patients feeling wary.
For years, the healthcare industry has wrestled with how much credit to give review sites such as Yelp and Google Places. But today, with so many patients turning to healthcare-specific review sites like Healthgrades and RateMDs, and the growing presence of healthcare providers on Facebook, there’s no denying the importance of online reviews and social media. In fact, according to statistics provided by the Mayo Clinic Health Care Social Media List and American Hospital Association, 41 percent of people said social media would affect their choice of a specific doctor, hospital or medical facility.
So, how do you improve online reviews along with your online reputation? Here are a few of the best practices for private practice doctors:
By: Julianne Filion | On: September 15, 2015

From calming anxious patients and comforting those in pain to managing complex procedures, tackling paperwork and answering countless questions, nurses are among the hardest working professionals in the industry. These everyday superheroes often sacrifice weekends, holidays and family time to care for those in need.
Call us crazy, but we think nurses deserve more than a week of appreciation. To help boost morale and improve employee satisfaction, here are a few easy ways to say “thank you!” to your nursing staff the other 51 weeks of the year:
By: Bethany Nock | On: September 10, 2015

As hospital administrators know, perhaps better than anyone, hospitals are complex organizations. Communication is a constant challenge, and it can take several months to implement even the smallest process change. After all of the paperwork, training and follow-up reviews, you may begin to question whether your amendments are truly improving the workspace, or simply adding more madness to the mayhem.
However, while failure to comply with some procedures, such as organizing supplies, may be a source of frustration, other procedures, such as those focused on patient-centered care, can have a major impact on your hospital’s success.
Here are a few ways you can improve patient-centered care in your hospital environment, and make sure it sticks.
By: Julianne Filion | On: September 8, 2015
 It’s one of the first procedures you learned in nursing school and, for many nurses working in a hospital environment, it can be one of the most common tasks you perform each day. IV starts have become so routine, you could probably do them in your sleep—though it’s likely frowned upon in most institutions. When it comes to starting IVs, you’re a seasoned pro.
It’s one of the first procedures you learned in nursing school and, for many nurses working in a hospital environment, it can be one of the most common tasks you perform each day. IV starts have become so routine, you could probably do them in your sleep—though it’s likely frowned upon in most institutions. When it comes to starting IVs, you’re a seasoned pro.
However, while IV procedures are commonplace for most nurses, they’re often a source of stress and anxiety for your patients. Even for those without needle phobia, being stuck with a needle and connected to an IV tube can be a frightening experience. Not to mention, patient anxiety has a tendency to stress even the most calm and collected professionals.
There is a solution, though. Here are a few reasons why you should consider adding topical anesthetics to your institution’s IV kits:
By: Bethany Nock | On: September 3, 2015
 There are plenty of things that change amidst the transition from childhood to adulthood. You no longer cry when your scoop of ice cream tumbles to the concrete, for example. And, more than likely, you no longer need the security of a teddy bear nightlight to ward off bad dreams. However, just because you’re paying your own bills and willingly consuming spinach doesn’t mean you’re suddenly immune to the pain and anxiety of a visit to the doctor.
There are plenty of things that change amidst the transition from childhood to adulthood. You no longer cry when your scoop of ice cream tumbles to the concrete, for example. And, more than likely, you no longer need the security of a teddy bear nightlight to ward off bad dreams. However, just because you’re paying your own bills and willingly consuming spinach doesn’t mean you’re suddenly immune to the pain and anxiety of a visit to the doctor.
There’s a common misconception in the medical world that adults don’t need to be numbed before a vaccination, or talked through an IV start, because they’re mature and experienced enough to simply “deal with it.” However, though they may not feel it appropriate to voice their concerns, adults can benefit from comfort measures just as much as children.
Here are three reasons healthcare providers should consider increasing patient comfort measures for adults, too:
By: Julianne Filion | On: September 1, 2015

When someone asks you about your workday, how often do you respond “busy,” “crazy” or “absolutely nuts”? It’s commonly known nurses are among the busiest and hardest working professionals in the industry.
But, while much of your job requires the ability to thrive in a fast-paced environment, there are plenty of timesaving tricks to help you make the most of each day. Here are our top five recommendations of timesavers:
By: Bethany Nock | On: August 27, 2015

“To cure sometimes, to relieve often, to comfort always.”
This quote, often attributed to Hippocrates, perfectly summarizes the mission statement of physicians worldwide. You strive, everyday, to cure ailments and relieve your patients’ symptoms, but success in these areas often depends on factors beyond your control. Relieving anxiety through patient comfort measures, on the other hand, is always within your power.
Unfortunately, in an effort to treat patients efficiently, and free up bed space, patient comfort sometimes falls to the wayside. Although you may have every intention of providing your patients with a comfortable experience, your ultimate goal is likely to treat as many people as possible within each shift.
While implementing additional patient care methods to your work as a doctor seems counterproductive to your goal of treating as many people as possible, there are plenty of methods to ensure patient comfort without adding to care time or impacting efficiency. Here are our top three suggestions:
By: Bethany Nock | On: August 25, 2015
You can’t open a paper, flip on a television or pull up your preferred news app without being bombarded with the phrase “rising cost of healthcare.” For those of us in the healthcare field, this concern is nothing new. After all, physicians have been navigating the costs of healthcare since the first day of med school. Not to mention, running your own private practice comes with its own fair share of financial concerns. But, as government mandates tighten purse strings and insurance changes force patients to become more cognizant of costs, private practices are under increased pressure to significantly decrease spend.
Luckily, there are several ways physicians can reduce costs without sacrificing quality of care. Here are our top three suggestions:
By: Bethany Nock | On: August 19, 2015
Imagine: After several days of apprehension and many sleepless nights, the appointment you’ve dreaded has arrived. Years of needle phobia topped with too many experiences that lacked patient comfort measures, like topical anesthetic spray for injections beforehand, have left you fearful and stressed for even routine visits. You follow your orthopedist’s friendly office assistant into a brightly-lit examination room smelling of disinfectant, and reluctantly remove your jacket. Your ailing shoulder is exposed, and now you’re one step closer.
“Doctor Jones will be with you shortly,” the staff member says. She closes the door as she disappears into the hall.
You begin to feel the familiar rush of anxiety. It starts in the pit of your stomach, and spreads up through your shaking hands. “Not again,” you say to yourself as you fight to suppress the overwhelming panic. Your throat becomes tight and your thoughts become fogged.
By: Bethany Nock | On: July 15, 2015
 As a child life specialist, when you’re called to a patient’s room, you never know what awaits on the other side of the door. In some cases, your services are needed to help calm the nerves of a toddler before she receives a vaccine. In other cases, you may walk in to find a hysterical child and his equally terrified parents. Sometimes you can bring a situation under control in a matter of minutes, but some take much, much longer.
As a child life specialist, when you’re called to a patient’s room, you never know what awaits on the other side of the door. In some cases, your services are needed to help calm the nerves of a toddler before she receives a vaccine. In other cases, you may walk in to find a hysterical child and his equally terrified parents. Sometimes you can bring a situation under control in a matter of minutes, but some take much, much longer.
By: Bethany Nock | On: June 17, 2015
 For private practice office managers, hiring and recruiting is a time-consuming, expensive and, quite frankly, frustrating endeavor. From finding the right talent, to ensuring new hires are properly trained, getting the right employees in place requires a great deal of business resources. Not to mention, it’s pricey. It costs 20 percent of a worker’s $50,000 salary to replace them, according to the Center for American Progress.
For private practice office managers, hiring and recruiting is a time-consuming, expensive and, quite frankly, frustrating endeavor. From finding the right talent, to ensuring new hires are properly trained, getting the right employees in place requires a great deal of business resources. Not to mention, it’s pricey. It costs 20 percent of a worker’s $50,000 salary to replace them, according to the Center for American Progress.
By: Bethany Nock | On: May 14, 2015
 Most of us are accustomed to seeing customer experience surveys from businesses like cable companies, retailers and automotive service centers. Days after you’ve purchased a product or paid for a service, you’ve probably received an email or automated phone call asking you to rank your satisfaction and share your comments. For many years, businesses have relied on customer feedback to measure success and improve processes. Today, however, you’ll begin seeing surveys from an unlikely source: your hospital.
Most of us are accustomed to seeing customer experience surveys from businesses like cable companies, retailers and automotive service centers. Days after you’ve purchased a product or paid for a service, you’ve probably received an email or automated phone call asking you to rank your satisfaction and share your comments. For many years, businesses have relied on customer feedback to measure success and improve processes. Today, however, you’ll begin seeing surveys from an unlikely source: your hospital.
By: Julianne Filion | On: April 8, 2015

For patients of any age, a trip to the hospital can be uncomfortable. However, for pediatric patients, it can be especially traumatic. In addition to the reason for their visit, which is likely stressful on its own, they’re introduced to an environment full of unusual sights and sounds. Depending on their age, they may have unpleasant memories of previous hospital visits. Not to mention, television shows and movies don’t exactly portray hospitals as a bright and cheerful space.
By: Bethany Nock | On: November 19, 2014
The fall season is here and winter is coming. This is time for the flu, but the exact timing and duration of flu seasons vary. Typically seasonal flu outbreaks begin as early as October. However the peak time for flu activity is between December and February.
By: Bethany Nock | On: November 19, 2014

A generation ago, spring meant baseball, fall signaled football season and winter brought basketball. Summer vacation was filled with impromptu kickball and badminton games. Times have changed. From an early age, children play and practice their sports year-round.
By: Bethany Nock | On: October 6, 2014
 In the fast-paced environment of the emergency room, every second counts. From sprained ankles to minor lacerations to heart attacks, ER nurses are on the front line, and under pressure to provide care that is appropriate, efficient and compassionate.
In the fast-paced environment of the emergency room, every second counts. From sprained ankles to minor lacerations to heart attacks, ER nurses are on the front line, and under pressure to provide care that is appropriate, efficient and compassionate.
By: Bethany Nock | On: September 29, 2014
 “Is this going to hurt?” Nurses have been asked the question time and time again. When it comes to easing patient anxiety, the responsibility usually falls on nursing professionals.
“Is this going to hurt?” Nurses have been asked the question time and time again. When it comes to easing patient anxiety, the responsibility usually falls on nursing professionals.